Choosing a Failure to Launch Recovery Program

Key Takeaways for Decision Making
- Assessment Scoring: If safety or daily functioning is severely impacted, prioritize residential care; for those needing flexibility for work/school, outpatient is often sufficient.
- Success Factors: Programs lasting 60–90 days with active family involvement show significantly higher completion rates (up to 83.2%).
- Immediate Action: Schedule a consultation to discuss privacy protocols and integrated care for co-occurring conditions.
Understanding Failure to Launch Syndrome
What Drives the Inability to Launch?
Before selecting a failure to launch recovery program, it helps to understand what holds young adults back from stepping into independence. To gauge the root causes, consider this practical self-assessment:
- Do I struggle to start tasks without reminders?
- Am I anxious about making decisions or leaving my comfort zone?
- Do setbacks feel overwhelming or impossible to recover from?
These patterns often signal deeper barriers beyond simple motivation. Research points to several core drivers, specifically executive function challenges—such as difficulty with time management, organization, or initiating daily activities. These aren’t just personality quirks; they are skills that require targeted, real-world practice to develop effectively.3
Anxiety and depression also play a major role, often causing avoidance or a sense of paralysis about the future. Recent studies highlight that for a large portion of young adults, mental health concerns are at the heart of the inability to launch, rather than a lack of ambition.1 Furthermore, social factors matter; lacking supportive mentors or positive peer connections increases the risk of feeling isolated. One national survey found 40% of young people grow up without a mentor, which can limit confidence and resilience.9
This approach is ideal for those who want flexible, discreet support that adapts to individual strengths and barriers. For those interested in programs that address multiple underlying factors, the next section will explore how co-occurring conditions can impact recovery.
Co-Occurring Conditions That Complicate Independence
Before choosing a failure to launch recovery program, it is essential to recognize how co-occurring conditions—when more than one mental health or behavioral challenge is present—can make independence feel even more out of reach. Use the following checklist to identify potential overlapping issues:

- Mood Instability: Frequent mood swings or ongoing anxiety.
- Focus Issues: Trouble focusing or symptoms of ADHD.
- Trauma History: Unresolved symptoms of past trauma.
- Daily Functioning: Significant struggles with basic daily tasks.
Studies reveal that over 50% of young adults with substance use concerns also live with another psychiatric condition, such as depression, anxiety, or ADHD.1 When these co-occurring conditions are present, they tend to interact—sometimes magnifying each other's impact. For example, untreated anxiety may worsen avoidance behaviors, while executive function difficulties can increase frustration and self-doubt in daily tasks.
Industry leaders find that the most effective recovery programs offer integrated care, bringing together specialists, mental health clinicians, and medical providers to address all needs at once.1 This solution fits individuals seeking a recovery journey that adapts to unique strengths and challenges, rather than a one-size-fits-all model. Prioritize programs that are discreet, respect privacy, and can coordinate care for co-occurring conditions.
Evidence-Based Treatment in Failure to Launch Recovery Programs
Cognitive-Behavioral Therapy and Skill Development
A practical checklist can help readers evaluate if cognitive-behavioral therapy (CBT) and skill-building should be at the core of their search for a failure to launch recovery program. When vetting providers, look for the following:
- Structured Sessions: Does the program offer structured CBT sessions (individual or group)?
- Real-Life Application: Is there a focus on practicing skills like time management in everyday settings?
- Measurable Goals: Does the program use measurable goals and track progress collaboratively?
"Studies show that nearly 60% of effective young adult programs deliver a psychotherapeutic intervention such as CBT, and that it works especially well for depressive symptoms, anxiety, and general psychological distress."3
CBT promotes emotional intelligence and coping skills, which are essential for building resilience and facing challenges that come with adulthood.7 Typically, 11 to 16 CBT sessions are needed for about half of clients to experience significant improvement.8
Skill development goes hand in hand with therapy. Research confirms that executive function challenges require real-world, repeated practice, not just abstract discussion.3 Programs that combine therapy with hands-on coaching, mentoring, and personalized goal-setting give participants the best chance for long-term change. This approach works best when privacy and adaptability matter, and when a young adult prefers practical support that fits into their life discreetly.
Family Involvement as a Success Multiplier
A quick assessment can help families decide how actively they want to be involved in a recovery program. Ask yourself: Would regular, guided family sessions be manageable with everyone’s schedules? Are there unresolved patterns at home—like miscommunication or enabling—that could affect progress?
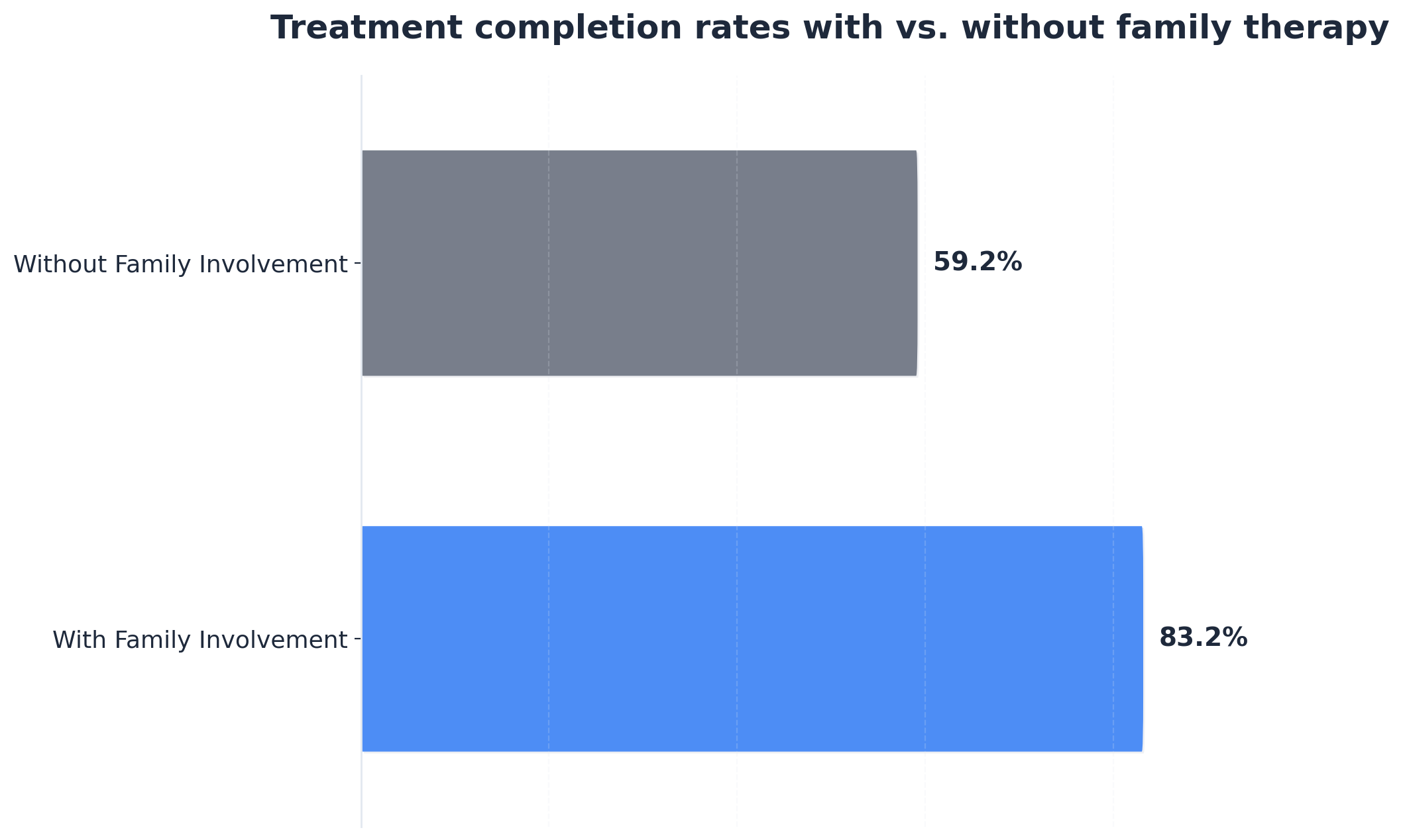
| Treatment Approach | Completion Rate | Impact |
|---|---|---|
| Standard Program (No Family Therapy) | 59.2% | Baseline outcomes. |
| Program with Family Participation | 83.2% | Significantly higher success; creates a network of accountability.2 |
Research shows that programs with robust family involvement consistently see better outcomes. Each additional family session increases the odds of finishing treatment by 1.4 times.2 This isn’t just about parental oversight; it’s about creating a network of encouragement. Family involvement can be as simple as participating in occasional check-ins or working with a therapist to develop healthier communication habits.
This strategy suits families who want their young adult’s recovery journey to be collaborative but discreet. Many modern programs now offer remote or flexible scheduling for family sessions, making it easier for busy households to participate. If you or your loved one would benefit from additional guidance, organizations like the National Alliance on Mental Illness (NAMI) provide resources for families seeking support.
Evaluating Program Structure and Duration
Why Timeline Matters for Measurable Change
A simple decision tool can help families and professionals assess whether a program’s timeline aligns with their goals. When reviewing options, verify the following:
- Does the program clearly outline short-term milestones and longer-term expectations?
- Are there regular progress reviews built into the schedule?
- Can the duration be adjusted to match changing needs?
Timeline is more than a calendar entry in failure to launch recovery programs—it’s a core indicator of sustainable progress. Studies reveal that programs lasting at least 60–90 days are significantly more likely to deliver measurable improvements in independence, executive function, and mental health stability.3 Shorter interventions often don’t provide enough time for lasting change, especially when addressing complex issues like co-occurring conditions.
Industry experts recommend choosing programs that offer ongoing assessment and the flexibility to extend support if needed, as recovery isn’t always linear.1 This path makes sense for those who seek visible, trackable results and want to avoid the frustration of starting over.
Flexibility vs. Structure: Finding Balance
When evaluating programs, it’s common to wonder how much flexibility is appropriate versus how much structure is needed. Use this practical assessment to determine the right fit:
Click to view Structure Assessment Questions
- Does the program provide a clear daily schedule but allow room for adjustments if stress or health needs shift?
- Can therapy or skill-building sessions be rescheduled or delivered virtually without penalty?
- Is there a process for regularly updating goals based on changing circumstances?
Research shows that young adults achieve the best outcomes when programs combine reliable routines with the ability to tailor interventions as needs evolve.3 Rigid, one-size-fits-all models may leave participants feeling boxed in, while overly loose programs risk losing momentum. The most effective recovery environments provide predictable touchpoints—such as weekly check-ins—while also adapting to setbacks. This approach is ideal for individuals who value privacy and want support that fits discreetly around school, work, or family obligations.
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.
Critical Questions for Failure to Launch Recovery Programs
When evaluating therapeutic programs for young adults, distinguishing between substantive offerings and marketing rhetoric is essential. Selecting the right failure to launch recovery program requires careful evaluation beyond surface-level promises. The following table outlines critical areas to investigate during your consultation to ensure the program aligns with your specific needs.
| Category | Questions to Ask | What to Look For |
|---|---|---|
| Treatment Planning | How do you conduct initial assessments and how often are care plans updated? | Genuine customization that adjusts as the client evolves, rather than rigid protocols. |
| Clinical Expertise | What are the specific credentials of the clinical team? | Training in young adult development and evidence-based modalities like CBT or DBT. |
| Family Role | How do you facilitate communication while respecting boundaries? | Clear philosophies on family therapy sessions and progress updates. |
| Lifestyle Integration | What are the policies on technology, employment, or education? | Support for gradual reintegration into community activities rather than total isolation. |
| Aftercare | What transition strategies and alumni support are available? | Resources and coping mechanisms established before the program ends. |
Building Your Young Adult's Path Forward
Once you've asked the critical questions about treatment approaches and outcomes, the next step is translating those answers into a concrete recovery plan. Recovery represents a journey of growth and self-discovery, particularly for young adults navigating the transition to independence. Creating a sustainable path forward requires balancing structure with flexibility, allowing space for personal development while maintaining essential support systems.

Successful outcomes depend on integrating treatment insights into daily life. This means establishing routines that support wellness—consistent sleep schedules that honor circadian rhythms, regular physical activity like morning walks or yoga, and reflective practices such as journaling to process emotions. Building healthy relationships involves learning to identify supportive connections, setting boundaries with people who trigger unhealthy patterns, and practicing vulnerability with trusted individuals.
Young adults also develop practical coping strategies, including:
- Grounding Techniques: Methods like the 5-4-3-2-1 sensory exercise for anxiety.
- Communication Skills: Tools for expressing needs clearly and assertively.
- Self-Regulation: Practices such as breathwork or progressive muscle relaxation.
The path forward should address underlying factors that contribute to behavioral health challenges, including trauma, anxiety, or depression. Comprehensive care considers the whole person, not just immediate concerns, creating foundations for long-term wellness. For example, a young adult struggling with substance use might discover that unresolved social anxiety drives their behavior—addressing both issues simultaneously creates more durable change than focusing on substance use alone.
Family involvement plays a vital role in sustainable recovery. Open communication, appropriate boundaries, and shared understanding of the recovery process strengthen support networks. When families participate in the healing journey through family therapy sessions or educational workshops, young adults gain confidence knowing they have people who understand their experiences.
Building this path requires patience, commitment, and the right professional partnership—typically a treatment team including a primary therapist, psychiatrist if medication is appropriate, and case manager who coordinates care. Finding these professionals often begins with your insurance provider's directory, referrals from your primary care physician, or organizations like NAMI that offer local resources. The investment in finding providers who specialize in young adult development and who communicate collaboratively creates the foundation for meaningful, lasting change that extends well beyond the treatment period itself.
Frequently Asked Questions
What is the typical cost range for a failure to launch recovery program?
Costs for failure to launch recovery programs can vary widely depending on the level of care, location, and included services. Outpatient options—such as weekly therapy and skill-building—may cost less, while more intensive residential programs or those offering personalized, concierge-style support typically require a larger investment. Since each program’s pricing is influenced by duration, staff expertise, and whether family or medical services are included, it’s best to contact providers directly for current rates. Research shows that treatment length and ongoing assessment often shape total cost, as programs lasting 60–90 days tend to yield the most measurable outcomes 3. Financial assistance or payment plans may be available—ask each provider about options that protect your privacy.
How do I know if my young adult needs residential treatment versus outpatient support?
Deciding between residential treatment and outpatient support for a young adult depends on the intensity of challenges and the level of structure needed. Residential programs are often best when safety is a concern, daily functioning is severely impacted, or when multiple co-occurring conditions require round-the-clock care. Outpatient options can work well if the young adult is able to manage daily routines with some support and prefers a flexible, discreet approach. Research shows programs should be tailored to individual needs, with integrated care for mental health and substance use concerns when present 1. When in doubt, seek a professional assessment to determine the most supportive environment. For guidance, organizations like NAMI offer confidential consultations.
Can my young adult participate in a program while maintaining privacy from employers or peers?
Yes, many failure to launch recovery programs are designed to protect participants’ privacy, making it possible for young adults to engage in support discreetly. Options like virtual sessions, flexible scheduling outside of work or school hours, and strict confidentiality policies help ensure that information is not shared with employers or peers unless the participant chooses to disclose. Research highlights the growing success of online and remote interventions for young adults, offering a level of privacy that is both practical and effective 4. When considering a program, ask directly about confidentiality practices and how your information will be protected throughout the process.
What happens if my young adult refuses to participate in the program?
If your young adult is hesitant or refuses to participate in a failure to launch recovery program, it’s natural to feel concerned or frustrated. Research shows that resistance is often connected to anxiety, fear of change, or a desire for greater autonomy—not simply a lack of willpower 1. In these situations, it can help to explore non-confrontational conversations, express support without pressure, and offer choices rather than ultimatums. Sometimes, starting with a lower-intensity or virtual approach can ease worries about privacy or commitment 4. For additional guidance, organizations like NAMI and the JED Foundation offer resources to help families navigate motivation challenges and find professional support that respects everyone’s boundaries.
How can I tell if a program is truly evidence-based or just using buzzwords?
To determine if a failure to launch recovery program is truly evidence-based, look for transparent explanations of the therapies used—such as cognitive-behavioral therapy (CBT), motivational interviewing, or skill-building—and ask if results are measured with clear progress tools. Effective programs often cite research showing that nearly 60% of successful young adult interventions use structured psychotherapeutic approaches like CBT 3. Be cautious if a program relies on vague terms (like “holistic” or “transformational”) without mentioning specific, proven methods or measurable outcomes. Request data on client progress, and see if staff have relevant clinical credentials. If in doubt, consult organizations like NAMI for help vetting options.
What role should I play as a parent during my young adult's recovery?
Parents play a supportive, collaborative role during a young adult’s recovery journey. Research shows that when families participate in therapy or regular check-ins, treatment completion rates for failure to launch recovery programs rise dramatically—from 59.2% to 83.2% 2. The most helpful approach is to offer encouragement, maintain healthy boundaries, and respect the young adult’s privacy and autonomy. Instead of trying to solve every problem, focus on open communication and being available for guidance as needed. Programs often provide education for parents on how to foster independence without enabling old patterns. If you’re seeking extra support, resources like NAMI offer confidential advice for families navigating this process.
How do programs address neurodivergence like ADHD or autism in young adults?
Programs that address neurodivergence—such as ADHD or autism—in young adults are most effective when they offer personalized, strengths-based support. Many failure to launch recovery programs now integrate executive function coaching, social skills development, and therapies like cognitive-behavioral therapy (CBT), which research shows can help with emotional regulation and daily functioning 3. Industry leaders find that flexible, real-world practice and trauma-informed care are important for neurodivergent participants, as rigid routines or abstract advice often fall short. Consider this route if a young adult needs discreet, adaptable support that recognizes their unique learning style and sensory needs. For further resources, organizations like NAMI offer guidance on neurodivergent-friendly program options.
References
- Principles of Care for Young Adults With Co-Occurring Psychiatric and Substance Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC8276159/
- The Impact of Family Therapy Participation on Youths and Young Adults. https://pmc.ncbi.nlm.nih.gov/articles/PMC10160927/
- What Interventions Help Teens and Young Adults: Rapid Evidence Review. https://academyhealth.org/sites/default/files/Rapid_Evidence_Review_Behavioral_HealthJan2018.pdf
- An Online Intervention for 18–25–Year–Old Youth Whose Parents Have Mental Illness or Substance Use Problems. https://pmc.ncbi.nlm.nih.gov/articles/PMC9790290/
- Measuring Goal Progress Using the Goal-Based Outcome Tool. https://pmc.ncbi.nlm.nih.gov/articles/PMC11937847/
- Housing Interventions for Emerging Adults Experiencing Homelessness. https://pmc.ncbi.nlm.nih.gov/articles/PMC8372952/
- The Effectiveness of Cognitive-Behavioral Group Therapy Training on Emotional Intelligence and General Health. https://pmc.ncbi.nlm.nih.gov/articles/PMC5319290/
- Effectiveness of Cognitive Behavioral Therapy: An Evaluation Study. https://pmc.ncbi.nlm.nih.gov/articles/PMC3888554/
- Mentoring Impact: How Mentoring Shapes Young People's Lives. https://www.mentoring.org/mentoring-impact/
- Addiction Relapse Prevention - StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK551500/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



