How to Find the Right Substance Abuse Interventionist

Executive Summary: Intervention Best Practices
- Essential Prerequisites: Verified clinical credentials (CIP, AADC, LMHC) and adherence to non-confrontational, evidence-based ethical codes.
- Strategic Steps:
- Verify multidisciplinary credentials and trauma-informed training.
- Assess methodology alignment (collaborative vs. confrontational).
- Evaluate comprehensive support systems (pre-planning through aftercare).
- Final Outcome: A unified family system and a safely transported client engaged in a matched treatment program with long-term recovery support.
Understanding Substance Abuse Interventionist Standards
Credentials That Matter Beyond the Basics
Industry professionals know that not all credentials carry equal weight when evaluating a substance abuse interventionist. While baseline requirements such as a high school diploma or GED are common, standout interventionists go far beyond this, holding specialized certifications that reflect advanced competency and ethical commitment. For example, the Certified Intervention Professional (CIP) credential requires not just education, but 2,000 to 6,000 hours of supervised experience, 150 hours of focused coursework across intervention theory, substance use disorders, mental health, family systems, motivational interviewing, and additional domains like ethics and crisis intervention, plus facilitation of at least 10 interventions within three years6.
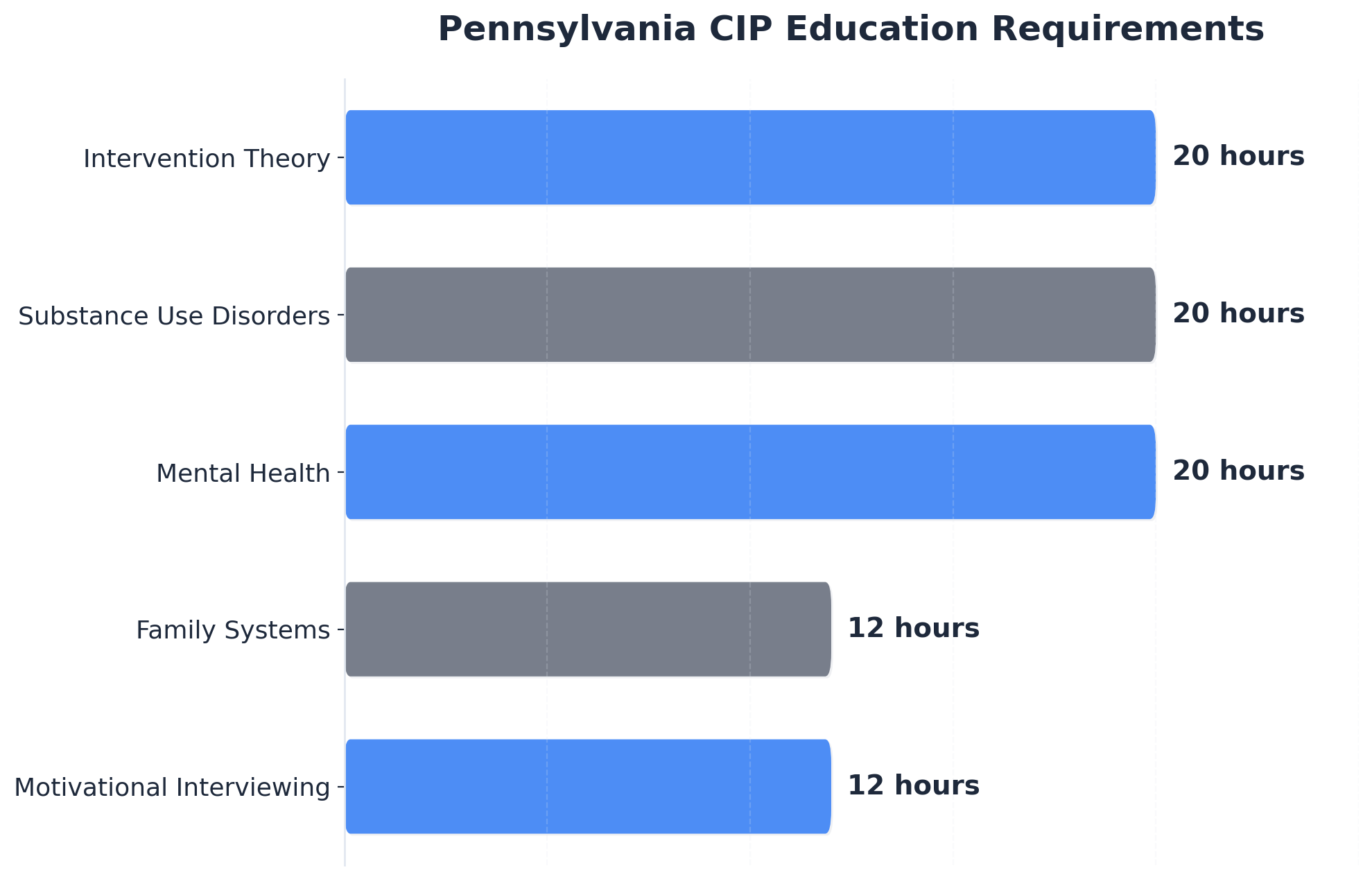
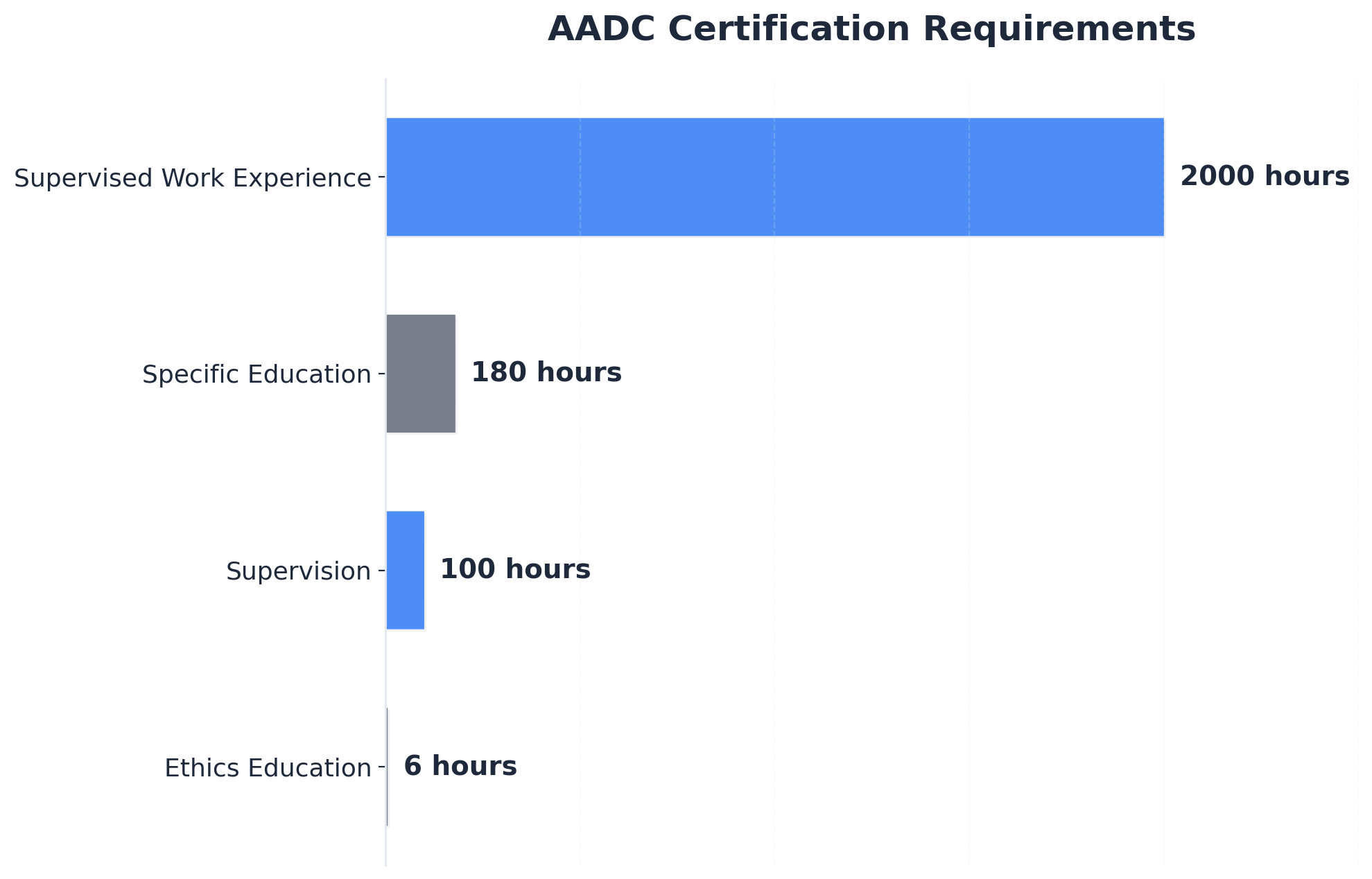
Advanced credentials such as the Advanced Alcohol & Drug Counselor (AADC) require a master’s degree, 2,000 hours of supervised work experience, 180 hours of specific education, and passage of a board examination5. These credentials indicate a practitioner’s ability to navigate complex family systems and co-occurring disorders—skills that are essential for high-stakes interventions.
Ethics also play a central role. Professional organizations like the Association of Intervention Specialists emphasize ongoing education, client welfare, and strict confidentiality standards7. The table below outlines key differences among common credentials to assist in rapid qualification comparison:
| Credential | Education Required | Supervised Experience | Ethics Training | Additional Requirements |
|---|---|---|---|---|
| CIP | 150 hours | 2,000–6,000 hours | Yes | 10 interventions, exam |
| AADC | 180 hours (Master’s) | 2,000 hours | Yes | Exam |
Research shows that higher credentialing aligns with improved intervention outcomes and greater family trust3. Next, it’s important to distinguish between evidence-based and confrontational intervention models.
Evidence-Based Models vs. Confrontation
Distinguishing between evidence-based intervention models and confrontational approaches is a crucial step for any professional seeking effective outcomes. Evidence-based models, such as the ARISE or Invitational models, rely on collaboration, structured planning, and ongoing support. These approaches draw from established practices in motivational interviewing and family systems theory, prioritizing respect and open communication. Research shows that interventions targeting both practitioners and clients result in positive outcomes in 86% of studies reviewed, indicating the power of collaborative, evidence-driven strategies9.
Confrontational models, often associated with the Johnson Model, take a more direct and sometimes adversarial approach. While these methods historically gained attention for their directness, studies reveal that such approaches may increase feelings of shame or resistance, especially in individuals with co-occurring mental health challenges. Industry leaders find that evidence-based, non-confrontational models tend to reduce defensiveness and foster greater willingness to engage in treatment, particularly when family dynamics are complex or when a gentle, supportive tone is needed8.
| Model | Approach | Family Involvement | Typical Outcomes |
|---|---|---|---|
| Evidence-Based | Collaborative, planned | High | Higher engagement, lower relapse |
| Confrontational | Directive, adversarial | Variable | Mixed, potential for resistance |
Choosing a substance abuse interventionist who practices an evidence-based model is more likely to lead to sustained engagement and positive change. With a clear understanding of these approaches, the next step is to verify the credentials and training of potential interventionists.
Step 1: Verify Substance Abuse Interventionist Credentials
Multidisciplinary credentials strengthen intervention outcomes, particularly for complex cases involving co-occurring disorders or treatment-resistant presentations. The most effective intervention teams draw from diverse professional backgrounds to create comprehensive support systems. Key credentials to look for include:
- Certified Intervention Professionals (CIP): Specialists in the mechanics and ethics of intervention.
- Certified Recovery Coaches (CRC): Experts in peer support and long-term sobriety maintenance.
- Association of Intervention Specialists (AIS) Members: Professionals bound by rigorous ethical codes.
- Licensed Mental Health Counselors (LMHC) & Master of Social Work (MSW): Clinicians who bring distinct perspectives to case management and family systems.
Clinical depth matters when navigating severe mental health crises, eating disorders, or situations where individuals have previously declined help. Interventionists with backgrounds in clinical social work, addiction counseling, or nursing contribute specialized expertise that enhances case conceptualization and treatment matching. Those holding LMHC or MSW credentials offer particularly valuable clinical insight for cases involving trauma histories, personality considerations, or complex family systems dynamics that influence intervention planning and execution.
Professional development in trauma-informed care, motivational interviewing, and crisis de-escalation represents essential ongoing education within the field. These specialized approaches become critical when working with individuals experiencing acute distress or demonstrating ambivalence about change. The intervention landscape continues evolving as research reveals more effective methods for engaging people across different presentations—substance use disorders, eating disorders, digital addiction, and process addictions each require tailored clinical frameworks.
The absence of universal licensing requirements in intervention work makes professional affiliations particularly meaningful. Active membership in organizations like the Network of Independent Interventionists or the Association of Intervention Specialists signals commitment to ethical standards and continuing education requirements. These professional communities foster knowledge sharing around emerging best practices and maintain accountability structures that strengthen the field's credibility.
Population-specific experience significantly influences intervention effectiveness and treatment matching accuracy. Professionals who regularly work with adolescents understand developmental considerations that differ markedly from interventions involving executives or older adults. Similarly, eating disorder interventions require distinct clinical knowledge compared to substance use cases. Strong intervention practices develop deep expertise in specific populations while maintaining collaborative relationships with specialists for cases outside their primary focus areas.
Transparent discussion of credentials, specialized training, and relevant experience establishes the professional foundation necessary for effective collaboration with families. The most successful outcomes emerge when intervention teams clearly articulate their clinical approach, demonstrate familiarity with appropriate treatment resources, and outline comprehensive aftercare coordination—creating confidence in the process before families enter crisis moments.
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.
Step 2: Assess Methodology and Approach Fit
Evaluating Intervention Philosophy Alignment
When referring to or collaborating with a substance abuse interventionist, it pays to look closely at how their core philosophy matches the needs and values of the family and client. Not all interventionists approach their work the same way—some lean into collaborative, family-inclusive models, while others may follow more directive methods. This alignment matters because research shows that interventions rooted in collaborative care principles, such as the ARISE or Invitational models, help 75% of patients reach diagnosis and begin treatment within six months, compared to less than 25% with traditional approaches10.
"Philosophy alignment" in practice often means the interventionist is open about their methodology, welcomes input from referring professionals, and can articulate how their approach supports both immediate safety and long-term recovery. When there’s a strong match between the interventionist’s philosophy and the family’s communication style or cultural background, engagement and outcomes tend to improve.
It’s helpful to ask questions about how the interventionist involves family or support systems, addresses resistance without confrontation, and adapts to unique case dynamics. Industry leaders find that a clear, evidence-based philosophy not only builds trust but also reduces unnecessary conflict, which is critical during high-stakes interventions9.
Specialized Population Experience Matters
When considering a substance abuse interventionist for referral or collaboration, their direct experience with specific populations can make a measurable difference in outcomes. Professionals recognize that families and clients often face intersecting challenges—be it co-occurring mental health conditions, adolescent behavioral issues, or cultural and linguistic needs. An interventionist with a proven track record in the relevant clinical population will be more attuned to unique presentations and risk factors. For example, a practitioner who regularly works with adolescents is likely to adapt communication strategies and safety protocols for youth, while someone experienced in dual diagnoses will integrate mental health best practices alongside substance use intervention.
Research shows that 86% of interventions targeting both practitioner competence and patient-specific needs yield positive outcomes, highlighting the value of specialized expertise9. This means that matching the interventionist’s background to the client’s demographic, diagnostic, or cultural profile is not just a detail—it’s a major factor in safety, engagement, and long-term adherence.
| Specialized Population | Key Considerations |
|---|---|
| Adolescents/Young Adults | Developmental stage, family dynamics |
| Co-occurring Disorders | Mental health integration, safety plans |
| LGBTQ+ Individuals | Affirming care, cultural sensitivity |
| High-Profile/Executives | Discretion, complex family systems |
| Cross-Cultural Populations | Language, customs, community resources |
Selecting a substance abuse interventionist with this targeted experience supports both immediate intervention goals and broader recovery trajectories. Next, it’s important to assess the interventionist’s approach to pre-intervention planning and coordination.
Step 3: Evaluate Comprehensive Support Systems
Pre-Intervention Planning and Coordination
Thorough planning is the backbone of any effective intervention, especially when working with complex family systems and high-stakes clinical presentations. A skilled substance abuse interventionist begins by gathering detailed background information, including clinical history, risk factors, and family dynamics. This phase often includes confidential consultations with referring professionals, family members, and sometimes treatment providers to ensure a full picture of circumstances.

A clear plan is crafted that outlines each participant’s role, addresses potential triggers, and anticipates safety concerns. Research shows that interventions with structured, collaborative preparation—where practitioners and families are aligned—see positive outcomes in 86% of cases9. The interventionist will coordinate logistics such as meeting location, timing, and follow-up protocols to minimize surprises and maximize engagement. This step also involves preparing families for possible emotional reactions, resistance, or crisis behaviors, and reviewing contingency plans for scenarios like withdrawal, aggression, or refusal.
Collaboration is key. The interventionist should work closely with everyone involved, ensuring clarity around confidentiality, communication channels, and next steps if the person agrees—or declines—treatment. When all stakeholders are prepared and unified, the intervention process becomes safer, more effective, and less likely to escalate.
Post-Intervention Follow-Through Protocols
Ongoing support after an intervention is just as vital as the planning and event itself. A substance abuse interventionist who delivers best practices will establish clear follow-through protocols for the period immediately after the intervention and throughout treatment initiation. These protocols often include regular check-ins with both the client and family, updates to referring professionals, and structured communication plans to help everyone stay aligned as the recovery process unfolds.
Research shows that interventions targeting both practitioners and patients—especially when they include post-intervention support—produce positive effects in 86% of studies reviewed9. This highlights why structured follow-through is essential for maintaining momentum, addressing setbacks, and adapting care if new challenges arise. Industry leaders find that relapse rates can be lowered and family engagement sustained when there’s a transparent plan for ongoing monitoring, access to resources, and crisis management. In practice, this usually means scheduled calls or meetings, written progress updates, and protocols for crisis response if the situation escalates.
A well-designed post-intervention protocol also ensures seamless handoff to treatment providers, with the interventionist facilitating introductions and sharing relevant case information as allowed by confidentiality agreements. This continuous involvement supports both immediate stabilization and longer-term recovery goals.
Partnering for Successful Outcomes
The diverse credentials and specialized expertise within a professional intervention team translate directly into more effective family partnerships. When families work with interventionists who bring clinical training, recovery experience, and therapeutic insight, they gain access to multifaceted support that addresses the full complexity of behavioral health crises—not just the immediate intervention moment.
Effective partnerships begin with open communication and comprehensive coordination. Families bring invaluable insights about their loved one's history, triggers, and relationship dynamics, while interventionists contribute clinical expertise and proven strategies. Consider the following case example:
A family facing their son's escalating substance use worked with a team that included both a certified interventionist and a licensed mental health professional. The clinical perspective identified co-occurring anxiety that had been driving self-medication, while the family's input revealed specific relationship ruptures that needed repair. This exchange created a comprehensive understanding that shaped not just the intervention approach, but the treatment placement recommendation and family therapy framework—resulting in the young man's acceptance of care and sustained engagement through 90 days of treatment.
Research shows that interventions supported by unified family involvement achieve acceptance rates exceeding 85%—significantly higher than those with fragmented support systems. The most successful outcomes emerge when families actively participate in preparation while trusting professional guidance on methodology and timing.
In another situation, parents of a daughter struggling with an eating disorder initially disagreed on approach, with one parent favoring immediate residential placement and the other resisting any formal treatment. Through structured family preparation sessions, the intervention team helped align their messaging and address underlying fears. The unified front they presented, combined with the daughter's trust in the interventionist's eating disorder expertise, led to voluntary treatment entry and measurable progress in family communication patterns that had been deteriorating for years.
Ongoing collaboration extends well beyond the initial intervention through concierge-level coordination that traditional models don't provide. When interventionists offer 24-hour availability, case management during treatment transitions, and life coordination support, families gain a consistent professional partner throughout the recovery journey. This sustained partnership—whether through check-ins during the first challenging weeks of treatment, coordination with therapists and prescribers, or support during step-down transitions—helps navigate challenges, reinforce progress, and adjust support as needs evolve. One family working with round-the-clock case management reported that having immediate access to their interventionist during their son's difficult first month in residential care prevented two potential early discharges, ultimately supporting his completion of the full program and successful transition to outpatient care with family relationships intact rather than further fractured.
Frequently Asked Questions
What happens if the intervention doesn't result in immediate treatment acceptance?
If an intervention does not immediately result in the person accepting treatment, the process is far from over. A skilled substance abuse interventionist will have prepared the family and support system for this possibility, emphasizing that change often requires more than a single conversation. Studies reveal that positive outcomes can still occur through continued engagement, follow-up meetings, and maintaining supportive, non-confrontational communication strategies 9. It’s common for individuals to need time to process the intervention, reflect on the concerns raised, and consider their options. In these cases, the interventionist typically helps the family set healthy boundaries, provides resources, and offers ongoing coaching to maintain momentum. Recovery is a journey, and ongoing professional support can increase the likelihood of future treatment acceptance.
How do interventionists handle co-occurring mental health conditions during the process?
A substance abuse interventionist with advanced training will always screen for and address co-occurring mental health conditions as part of their process. This means collaborating with referring clinicians, reviewing relevant clinical history, and integrating evidence-based strategies that account for both substance use and mental health needs. Research shows that interventions targeting both practitioner competence and patient-specific needs—like dual diagnoses—yield positive outcomes in 86% of cases 9. During the intervention, the professional will avoid confrontational tactics that could escalate mental health symptoms, instead focusing on safety, communication, and linkage to comprehensive care. Coordinated planning and close communication with mental health professionals help ensure that the approach is both safe and responsive to the individual’s full clinical picture.
What's the typical timeline from initial consultation to intervention execution?
The timeline from initial consultation to intervention execution with a substance abuse interventionist usually spans several days to a couple of weeks. After the first call, the interventionist gathers detailed background information and coordinates confidential meetings with key family members or referring professionals. Research shows that collaborative care models—where preparation and communication are prioritized—help 75% of patients reach diagnosis and start treatment within six months, much faster than standard approaches 10. Most interventions are scheduled as soon as planning, participant preparation, and risk assessments are complete. Urgent cases may move faster, but thorough pre-intervention planning remains essential for safety and effectiveness.
Should family members expect ongoing support after the person enters treatment?
Family members should expect ongoing support after the person enters treatment, as it plays a vital role in long-term recovery outcomes. A substance abuse interventionist typically coordinates regular check-ins, progress updates, and provides resources for both families and clients during this transition. This ongoing involvement helps families adjust to new routines, understand treatment processes, and respond effectively to any setbacks or questions that arise. Research shows that interventions which include structured follow-through and family engagement have positive effects in 86% of cases, underscoring the importance of continued support 9. Maintaining this connection offers reassurance and helps sustain motivation on both sides.
How do interventionists coordinate with treatment facilities for seamless transitions?
A substance abuse interventionist coordinates with treatment facilities by acting as a bridge between the client, their family, and the chosen program. This typically starts with sharing relevant case information—always within confidentiality guidelines—so the treatment team understands the client's background, needs, and immediate risks. The interventionist will often facilitate introductions, confirm admission details, and arrange logistics such as transport and timing, all while keeping referring professionals and families updated. Research shows that interventions combining practitioner coordination with ongoing support yield positive outcomes in 86% of studies, highlighting the value of seamless handoffs 9. This collaborative approach means the client arrives at the facility supported and prepared, reducing anxiety and increasing the likelihood of successful treatment initiation.
What safeguards exist if the person becomes hostile or threatens violence during intervention?
If a person becomes hostile or threatens violence during an intervention, experienced professionals have safeguards in place before the meeting even begins. A substance abuse interventionist will assess risk factors during planning, including any past history of aggression or mental health crises. Safety protocols may include holding the intervention in a neutral, secure setting, arranging for immediate access to clinical or emergency support, and ensuring all participants know when to pause or exit if safety is at risk. Research shows that well-structured planning—including contingency strategies for crisis behaviors—greatly reduces the chance of escalation and helps protect everyone involved 1. Clear communication and boundaries are key, and the interventionist will guide the group on how to respond calmly and prioritize safety throughout the process.
References
- Intervention: Help a Loved One Overcome Addiction - Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/mental-illness/in-depth/intervention/art-20047451
- Association of Intervention Specialists (AIS). https://www.associationofinterventionspecialists.org/
- TAP 21: Addiction Counseling Competencies - SAMHSA. https://library.samhsa.gov/sites/default/files/sma12-4171.pdf
- About The ASAM Criteria. https://www.asam.org/asam-criteria/about-the-asam-criteria
- Advanced Alcohol & Drug Counselor (AADC) - IC&RC. https://internationalcredentialing.org/icrc-credentials/aadc/
- Certified Intervention Professional (CIP) - Pennsylvania Certification Board. https://www.pacertboard.org/certified-intervention-professional-cip
- AIS Code of Ethics. https://www.associationofinterventionspecialists.org/code-of-ethics/
- The Impact of Substance Use Disorders on Families. https://pmc.ncbi.nlm.nih.gov/articles/PMC3725219/
- Effect on Health-Related Outcomes of Interventions to Alter Practitioner-Patient Interaction. https://pmc.ncbi.nlm.nih.gov/articles/PMC1466743/
- Collaborative Mental Health Care: A Narrative Review. https://pmc.ncbi.nlm.nih.gov/articles/PMC9803502/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



