What Are the Different Types of Crisis Intervention?

Key Takeaways
- Assess the Urgency: Use the "Safety-Function-Time" scoring guide to determine if you need immediate 911 assistance, a mobile crisis team (within 60 minutes), or a scheduled concierge consultation.
- Select the Right Model: Match the intervention to the need—use SAFER-R for immediate stabilization of acute stress, and Roberts' Seven-Stage Model for complex, multi-layered family dynamics.
- Prioritize Continuity: Success relies on the "warm handoff." Ensure any crisis service you choose includes a coordinated transition to ongoing therapy or coaching to prevent future relapse.
- Immediate Action: If safety is not at immediate risk but distress is high, contact a mobile response team or private behavioral health advocate today to create a preemptive safety plan.
Understanding Crisis Intervention Fundamentals
Defining Crisis and Intervention Goals
Navigating a mental health emergency requires a clear understanding of the available support systems. There are various types of crisis intervention designed to meet you exactly where you are, whether that involves a sudden loss, trauma, or a significant life transition that temporarily disrupts your sense of stability. In the realm of behavioral health, the primary objective is to rapidly restore safety and control while mitigating the risk of long-term impact.
The work typically centers on stabilizing emotions, reducing immediate distress, and guiding an individual back to their baseline level of functioning. To clarify these aims, consider this quick assessment tool:
- Safety Check: Is the person’s safety at risk (to self or others)?
- Functionality Check: Are they unable to manage daily life due to emotional distress?
- Timing Check: Is there a need for urgent, short-term support before ongoing care can begin?
When any answer is “yes,” intervention goals should focus on safety, de-escalation, and building a bridge to further help. Many modern interventions achieve these targets in a discreet, adaptable manner—meeting people at home, work, or virtually. Research indicates that short-term crisis intervention helps reduce long-term impact and supports a return to mental wellness more effectively than standard care alone.1

When Crisis Support Becomes Essential
Recognizing the precise moment to seek professional support can be challenging, particularly when emotions run high or daily life feels unmanageable. To assist in this decision, review the following practical checklist:
Types of Crisis Intervention_Next-level-wellness:
- Routine Disruption: Persistent inability to perform basic routines (work, school, self-care).
- Emotional Withdrawal: Expressions of hopelessness or withdrawal from support networks.
- Behavioral Shifts: Sudden changes in mood, behavior, or communication styles.
- Safety Concerns: Risks such as thoughts of self-harm or harm to others.
- Escalation: Increasing substance use or engagement in risky behaviors.
When several of these signs are present, it is time to consider specialized crisis intervention. This approach is most effective when support is discreet, adaptable, and responsive—such as arranging in-home visits, telehealth sessions, or connecting with mobile teams.
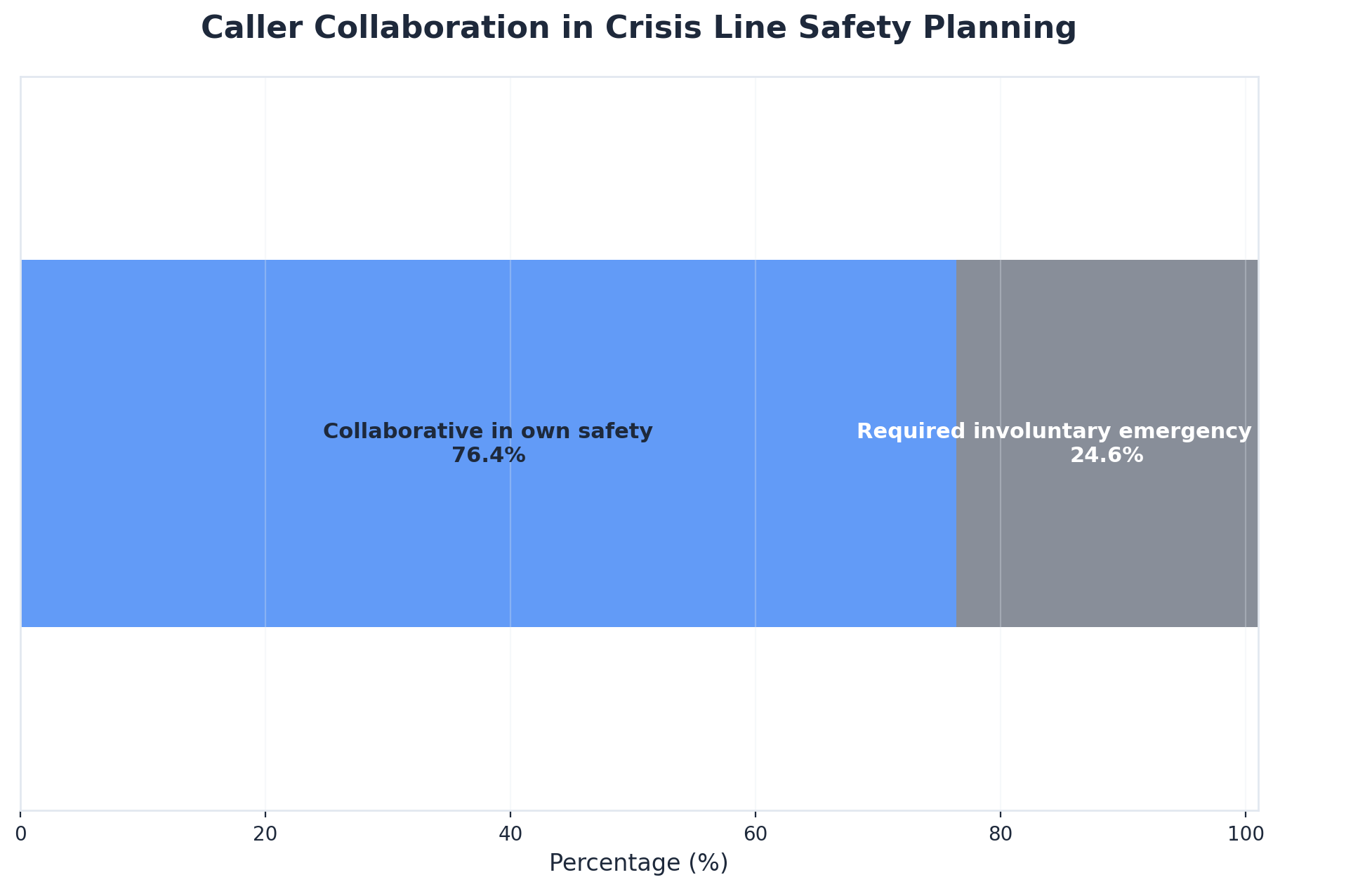
Studies reveal that over 76% of individuals who seek help through crisis hotlines are able to collaborate in creating a safety plan and remain safe in their preferred environment, highlighting the impact of timely, personalized intervention. If you or someone you know needs immediate help, national and local helplines are available 24/7.10
Evidence-Based Types of Crisis Intervention Models
The SAFER-R and Roberts Seven-Stage Models
When considering evidence-based types of crisis intervention, the SAFER-R and Roberts Seven-Stage Models are frequently utilized by behavioral health professionals. These frameworks guide individuals through acute emotional distress in a structured, supportive manner.
The SAFER-R model—Stabilize, Acknowledge, Facilitate understanding, Encourage coping, Recovery, and Referral—offers a concise roadmap. Industry leaders find SAFER-R helps clients regain a sense of safety and control faster than standard care, making it an ideal choice for those seeking discreet and flexible support1.
Conversely, Roberts’ Seven-Stage Model provides a granular process. It begins with a biopsychosocial and safety assessment, builds rapport, identifies the main problem, explores feelings, brainstorms coping strategies, creates a detailed action plan, and ensures follow-up care. This strategy suits situations where risk is uncertain or where a comprehensive approach is needed.5
ABC Model and Trauma-Informed Approaches
The ABC Model and trauma-informed approaches offer distinct pathways for crisis intervention, each emphasizing flexibility and respect for personal experience. To help you choose the appropriate path, consider the following decision tool:
Click to Reveal: Decision Tool for ABC vs. Trauma-Informed Care
- Opt for the ABC Model when the situation calls for structured, stepwise support—especially in educational or workplace settings.
- Choose Trauma-Informed Approaches if the person’s history suggests prior trauma, or when minimizing the risk of retraumatization is a top priority.
The ABC Model—A for Achieving rapport, B for Boiling down the problem, and C for Coping—guides professionals through building trust and collaboratively identifying coping strategies. This model works well in schools and community programs. In fact, 83% of public schools now offer individual-based interventions, which often use this type of stepwise support to address mental health needs discreetly.9
Trauma-informed crisis intervention prioritizes safety, empowerment, and choice. Rather than focusing solely on current symptoms, it asks, “What happened to you?” and adjusts responses to avoid triggers. This approach is ideal for those with complex behavioral health histories, as research highlights that trauma-sensitive care reduces the risk of retraumatization and supports lasting recovery.1

Mobile and Community-Based Types of Crisis Intervention
Mobile Response Teams and Alternative First Responders
Mobile Response Teams (MRTs) and alternative first responder programs have become standout options among the different types of crisis intervention. These are particularly valuable for people who prioritize privacy, flexibility, and rapid support in their own environment.
To help decide if this approach is right for you or a loved one, consider this practical checklist:
- Is there an urgent behavioral health or substance use crisis, but no immediate physical danger requiring police or EMTs?
- Would in-person, on-demand support at home, work, or in the community feel safer or more effective than going to an ER?
- Is discretion and a non-judgmental, therapeutic response a top priority?
If these sound familiar, mobile crisis teams often provide the right mix of adaptability and professional care. These teams are typically staffed by licensed clinicians and peer specialists who can de-escalate situations and connect individuals to ongoing services. For youth, research shows a 25% reduction in subsequent emergency department visits when a mobile crisis model is used.4
Alternative first responder programs go a step further by dispatching behavioral health professionals instead of law enforcement for mental health or welfare checks. This solution fits communities and families seeking to avoid criminal justice involvement and receive health-focused, trauma-informed support instead.6
Crisis Intervention Team Programs for Law Enforcement
Crisis Intervention Team (CIT) programs have transformed how law enforcement responds to behavioral health emergencies. These programs equip police officers with specialized training to de-escalate situations and connect individuals to appropriate care, rather than defaulting to arrest or hospitalization.
For readers considering the right types of crisis intervention, here is a quick assessment tool regarding CIT readiness:
- Training: Are law enforcement officers in your area trained in mental health crisis response?
- Partnerships: Does your community have partnerships between police, mental health providers, and hospitals?
- Diversion: Is there a track record of diverting individuals from jail to treatment?
The Memphis model, one of the most famous CIT frameworks, led to an 80% reduction in officer injuries during mental health calls—demonstrating how effective collaboration can improve safety for everyone involved.7
CIT programs also help families and professionals find support that is discreet and focused on health. If you’re unsure whether this option is available locally, organizations like NAMI can provide resources and connect you to CIT-trained officers.
Specialized Types of Crisis Intervention by Need
Suicidal Crisis and Safety Planning Interventions
Suicidal crisis and safety planning interventions are highly specialized types of crisis intervention focused on immediate risk reduction and establishing a clear, actionable path to safety. For anyone concerned about themselves or someone else, a practical tool—known as the Safety Planning Intervention (SPI)—can be life-saving.
This involves working collaboratively to identify warning signs, personal coping strategies, trusted contacts, and ways to limit access to means of self-harm. The plan is discreet, portable, and tailored to each person's unique lifestyle and preferences. This approach works best when the crisis is acute and the priority is to restore a sense of control and hope, rather than tackling root causes in the moment.
Industry research highlights that usual problem-solving methods are less effective during a suicidal crisis, so interventions must focus on immediate safety and practical coping steps. Lethal means counseling is another vital element, helping individuals and loved ones create a safer environment during vulnerable periods. These interventions are designed to be supportive and non-judgmental, making them especially valuable for professionals or families who want help that is both discreet and adaptable.8
Family-Based Crisis Support for Eating Disorders and Substance Use
Family-based crisis support has become a leading approach for addressing eating disorders and substance use, especially when a loved one is in acute distress. To help families navigate these situations, consider the following decision tool:
- Is the individual withdrawing from meals or routines?
- Are there major shifts in mood, secrecy, or physical health?
- Is substance use escalating despite previous support attempts?
Two primary frameworks support families in these scenarios:
These types of crisis intervention are ideal for families wanting adaptable, private support that fits their values and lifestyle. Both FBT and CRAFT can be delivered in-home or virtually, making them accessible and discreet. For ongoing guidance, organizations like Al-Anon, Nar-Anon, and local behavioral health teams offer further resources.
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.
Choosing the Right Crisis Support Path
Finding the right crisis support begins with understanding your unique situation and needs. Effective mental health crisis care is not one-size-fits-all, but rather a spectrum of options designed to match varying levels of need with appropriate intervention. Mental health emergencies range in intensity and nature, from severe anxiety episodes and major depressive episodes to active thoughts of self-harm or acute substance use challenges.
The path that works best depends on factors like symptom severity, available support systems, and personal preferences for care delivery. Empowering yourself with knowledge of these options enables you to select the most appropriate resource when crisis strikes.
For immediate life-threatening situations—such as active suicidal intent with a plan or severe psychotic episodes—emergency services provide critical intervention through 911 or hospital emergency departments. However, individuals experiencing moderate crisis symptoms, such as escalating distress without immediate danger, often benefit from less intensive options that offer professional support while maintaining privacy and flexibility.
Crisis hotlines like the 988 Suicide and Crisis Lifeline connect you with trained counselors 24/7, providing immediate emotional support and guidance, with average wait times under two minutes. Mobile crisis teams can come to you, offering assessment and intervention in familiar surroundings, with studies showing that approximately 70-80% of mobile crisis encounters successfully divert individuals from emergency department visits.
Beyond traditional emergency services, technology has transformed crisis care options and expanded accessibility. Virtual crisis services now allow individuals to receive professional support from home through secure video or phone sessions, with user satisfaction rates exceeding 85% in recent surveys. These options often appeal to those seeking discreet care that adapts to demanding schedules, as well as individuals in rural areas where in-person crisis services may be limited.
Consider your comfort level with different settings, the urgency of your needs, and whether you prefer in-person or remote support when selecting your crisis pathway. Resources like the 988 Suicide and Crisis Lifeline (call or text 988) and SAMHSA's National Helpline (1-800-662-4357) offer free, confidential guidance in choosing appropriate care pathways. Remember that matching your specific crisis situation with the right level of care—whether that's a supportive phone conversation, a mobile team visit, or emergency intervention—maximizes the likelihood of effective support and sustainable recovery.
Let's Create Lasting Change, Together
At Next Level Wellness & Behavioral Health, we provide premier concierge behavioral healthcare and highly personalized support for individuals and families navigating substance use, mental health challenges, eating disorders, complex life transitions, and more.
Our discreet, concierge, and expert-driven approach ensures dignity, compassion, and results-oriented care whether at home, in transit, or across multiple levels of treatment.
For support that meets you right where you are—anytime, anywhere—connect with us today.
Frequently Asked Questions
How much does private crisis intervention support typically cost compared to traditional emergency services?
Private crisis intervention support is typically a personalized, concierge-level service that can be scheduled at home, virtually, or in discreet settings. While precise costs are not universally published, industry data shows that community-based crisis care is significantly less expensive than traditional emergency services, such as hospital ER visits or law enforcement involvement. For example, community-based mental health treatment can cost about a third of what incarceration with mental health support would cost annually. This path suits individuals or families who want adaptable and confidential care, and may also reduce unnecessary hospitalization costs. For help finding the right fit, professional referral services or local behavioral health agencies can guide you.7
Can crisis intervention services maintain confidentiality for professionals concerned about career impact?
Absolutely—confidentiality is a cornerstone of crisis intervention services, especially for professionals who may worry about the impact on their reputation or career. Providers are legally and ethically required to protect personal health information, and many types of crisis intervention are designed to be discreet, including private in-home sessions, secure telehealth, or mobile teams that arrive without uniforms or marked vehicles. Only in extreme situations—such as immediate safety threats—are providers obligated to share limited information with emergency contacts or authorities. For those seeking the most private support, concierge behavioral health services and professional referral networks can tailor care to fit your confidentiality needs. For guidance, organizations like NAMI or professional medical associations can help you find trusted, discreet resources.1
What happens if someone refuses crisis intervention when family members believe it's necessary?
When someone declines crisis intervention—even if family members feel it's urgent—professionals respect their autonomy unless there is an immediate safety risk. Involuntary intervention is generally reserved for situations where a person poses a danger to themselves or others, following strict legal and ethical guidelines. Many types of crisis intervention include family support and coaching, helping loved ones communicate effectively, set boundaries, and encourage voluntary help over time. If safety is a concern, contacting a crisis team or national helpline can guide next steps. Family members can also seek support from resources like NAMI or Al-Anon for ongoing encouragement.1
How quickly can a mobile crisis team respond, and what areas do they typically serve?
Mobile crisis teams are designed to respond rapidly—many aim to arrive within 60 minutes of a call in urban and suburban areas, with some programs even faster depending on local resources. Rural response times may vary but teams still prioritize urgent outreach and can often offer telehealth support while en route. These teams usually serve entire counties or metro regions, with some expanding to statewide coverage as demand grows. This solution fits individuals seeking immediate, discreet support at home, work, or in the community, and research shows such teams reduce unnecessary ER visits by 25% for youth in crisis.4
What's the difference between calling a crisis hotline and requesting an in-person crisis intervention?
Calling a crisis hotline connects you immediately to trained professionals who offer support, risk assessment, and help creating a safety plan over the phone—often within minutes and available 24/7. This method is highly accessible, private, and allows most people to remain safely in their environment; in fact, over 76% of callers are able to collaborate on a safety plan without needing further intervention. In-person crisis intervention, on the other hand, involves sending a clinician or crisis response team to your location for direct support, de-escalation, and hands-on planning. This approach works best when the situation requires immediate physical presence or when phone support isn’t enough to ensure safety.10
How do crisis intervention services coordinate with ongoing therapy or treatment programs?
Crisis intervention services are designed to bridge immediate support with ongoing therapy or treatment programs, ensuring a seamless transition for individuals in need. After stabilizing the crisis, professionals typically coordinate with the person’s existing therapist, psychiatrist, or care team—always with consent—to communicate what occurred, share safety plans, and recommend next steps. This collaborative approach helps maintain treatment momentum and reduces the risk of gaps in care. Research shows that continuity between crisis support and ongoing therapy leads to better long-term outcomes and fewer repeat emergencies. For those without a current provider, crisis teams can offer referrals to trusted behavioral health specialists, making sure follow-up is both discreet and tailored to personal needs.1
Are there specialized crisis interventions for young adults experiencing failure to launch or digital addiction?
Yes, there are specialized types of crisis intervention for young adults navigating challenges like failure to launch or digital addiction. These interventions often blend behavioral health coaching, family involvement, and practical skill-building—delivered in ways that respect privacy and individual pace. For example, some programs use motivational interviewing and structured family support to address digital overuse, while others provide in-home or virtual coaching to help young adults develop independence. Research shows that family-based approaches can significantly boost engagement and reduce dropout, especially for youth and young adults. For discreet, adaptable support, concierge-style services and professional referrals can help tailor the intervention to unique lifestyle needs.3
References
- Crisis Intervention - Short-term management technique. https://www.ncbi.nlm.nih.gov/books/NBK559081/
- Chapter 3—Family Counseling Approaches. https://www.ncbi.nlm.nih.gov/books/NBK571088/
- Family-Based Treatment for Adolescent Eating Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC2828763/
- Alternative First Responder Models Can Help Youth in Crisis. https://csgjusticecenter.org/2023/08/22/alternative-first-responder-models-can-help-youth-in-crisis/
- Clinical Practice Guidelines for Assessment and Management of Crisis. https://pmc.ncbi.nlm.nih.gov/articles/PMC10096203/
- Alternative Emergency Response: Insights from the Field. https://govlab.hks.harvard.edu/insight/how-jurisdictions-are-approaching-alternative-emergency-response-implementation/
- Crisis Intervention Team (CIT) Programs. https://www.nami.org/advocacy-at-nami/crisis-intervention/crisis-intervention-team-cit-programs/
- Brief interventions for managing suicidal crises. https://afsp.org/brief-interventions-for-managing-suicidal-crises/
- The Landscape of School-Based Mental Health Services. https://www.kff.org/mental-health/the-landscape-of-school-based-mental-health-services/
- The Effectiveness of Crisis Line Services: A Systematic Review. https://pmc.ncbi.nlm.nih.gov/articles/PMC6978712/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



