5 Steps for Staging an Intervention for Depression

Key Takeaways
- Essential Prerequisites: A licensed professional facilitator, a private and neutral location, and a unified family team.
- Core Steps:
- Identify critical warning signs beyond simple sadness.
- Assemble a strategic team of supportive family members.
- Craft and rehearse non-judgmental, empathetic messages.
- Conduct the meeting in a safe environment.
- Secure commitment for a professional evaluation.
- Successful Outcome: A structured, compassionate pathway that guides your loved one toward professional treatment while preserving family dignity and relationships.
Recognizing When Staging an Intervention for Depression Is Needed
Critical Warning Signs Beyond Sadness
When considering staging an intervention for depression, it is vital to recognize that depression is far more than persistent sadness. Industry leaders highlight that warning signs often go beyond mood changes, especially in high-functioning adults or those accustomed to masking distress in professional or family roles. Readers might be wondering what truly marks a turning point for action. The answer often lies in a pattern of shifts across daily functioning and emotional expression, not just one-off bad days.
Key warning signs include marked withdrawal from social or family activities, a noticeable drop in work performance, or neglect of personal hygiene. Loss of interest in previously enjoyable activities, intense irritability, and persistent fatigue or sleep disturbances also signal depression’s deeper hold. If a loved one expresses feelings of worthlessness, hopelessness, or talks about being a burden, these are critical red flags.4
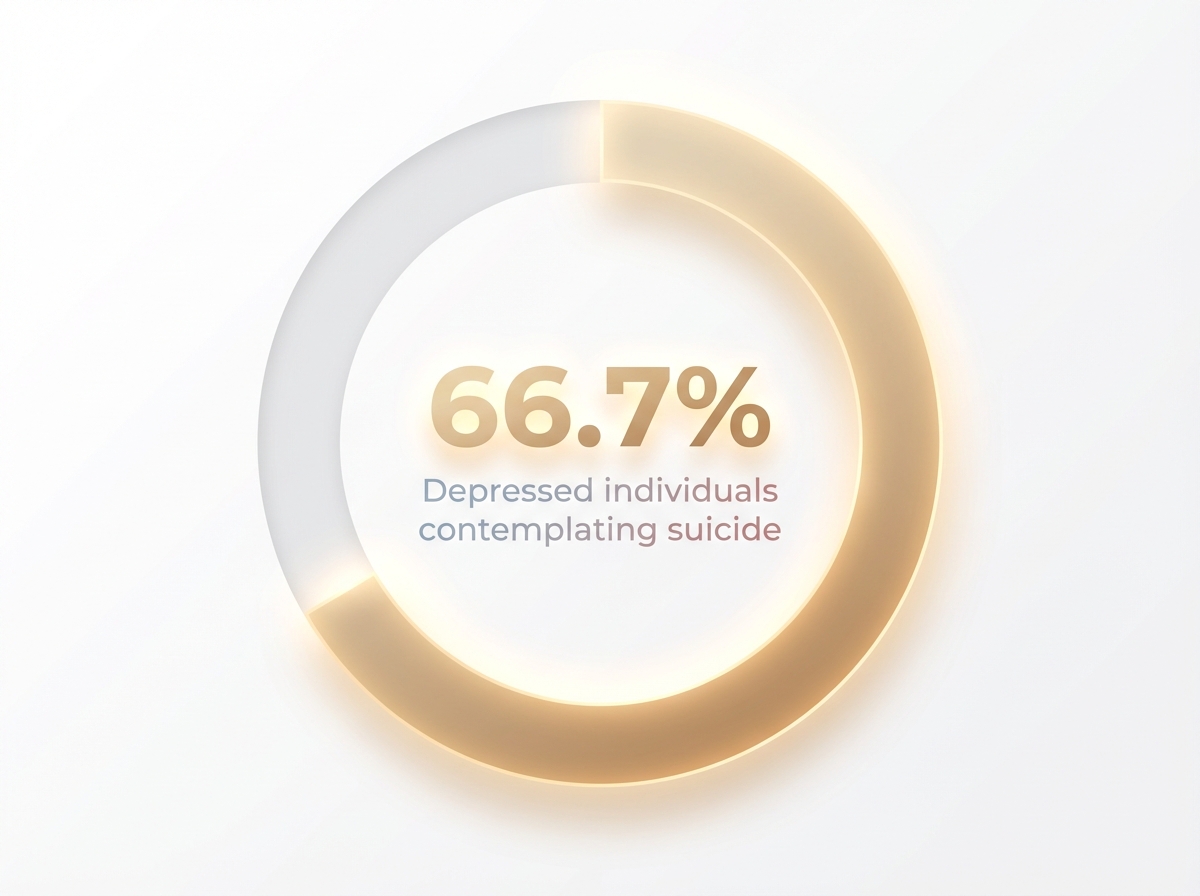
Most concerning are any signs of self-harm or thoughts of suicide—these situations require immediate professional support. Studies reveal that about two-thirds of people with clinical depression contemplate suicide, and between 10-15% may die by suicide, underscoring the importance of early recognition and intervention.4,10
Physical symptoms shouldn’t be ignored. Chronic pain, headaches, digestive problems, or unexplained aches may appear when depression is severe. These signs, combined with emotional changes, often represent the tipping point where compassionate intervention becomes essential. Recognizing these patterns empowers families to act before depression becomes a prolonged crisis. The next step involves understanding how support transitions into a structured intervention plan.
The Difference Between Support and Intervention
When discussing staging an intervention for depression, it is helpful to clarify what makes an intervention different from everyday support. Support often means checking in, offering a listening ear, or gently encouraging someone to seek help. These gestures play a crucial role, especially in the early stages of concern. However, when depression persists, deepens, or seriously disrupts daily life, more structured action may be needed.
Intervention steps in when support alone is no longer enough. Unlike casual encouragement, an intervention involves a coordinated effort—usually with multiple family members, friends, and a trained professional—to address the seriousness of the situation directly. The aim is not confrontation, but rather to create a safe, unified moment where concerns are communicated clearly, and a pathway to professional treatment is presented.5
A key distinction is in the intent and preparation. Support is ongoing and informal, often led by intuition. Intervention is planned, time-bound, and goal-oriented. It requires setting aside personal fears, aligning messages, and sometimes consulting with mental health experts to avoid blame or accidental escalation. The table below summarizes the main differences:2
As families move from support to staging an intervention for depression, recognizing this shift can help ensure that action matches the level of need. Next, it is essential to consider how to build the right intervention team for these sensitive situations.
Building Your Intervention Team Strategically
Selecting the Right Professional Facilitator
Selecting a professional facilitator is a foundational step when building an intervention team for depression. The right facilitator not only brings clinical expertise but also an understanding of family systems and the nuances of staging an intervention for depression. This role is typically filled by a licensed mental health professional—such as a psychologist, clinical social worker, or interventionist—who specializes in mood disorders and has experience guiding families through emotionally charged situations.
One key consideration is finding someone who is skilled at balancing empathy with structure. Research shows that interventions led by mental health professionals are more likely to result in treatment engagement, especially when the facilitator uses evidence-based strategies to keep the conversation focused and nonjudgmental. The facilitator should be adept at diffusing tension, managing strong emotions, and redirecting discussions if they begin to trigger shame or hopelessness.2
Experience with intervention models that avoid ultimatums and confrontation is particularly important, as these approaches reduce the risk of escalating distress. Credentials matter, but so does personal fit. Families often interview several professionals to find someone who communicates clearly and inspires trust. It is helpful to seek facilitators who are familiar with collaborative, family-centered approaches and who can provide references from similar cases. Choosing the right facilitator sets a supportive and safe tone for everyone involved.5
Choosing Family Members Who Strengthen the Message
Once a professional facilitator is onboard, selecting family members for the intervention team becomes a strategic process. When staging an intervention for depression, the goal is to assemble a group whose presence will be both reassuring and motivating. Research highlights that family environments marked by high “expressed emotion”—such as criticism, hostility, or over-involvement—can actually worsen depression symptoms and increase the risk of relapse. This makes it critical to choose participants who can share concern without judgment, and who naturally maintain calm, supportive energy.2
Ideally, the team should include family members with a close, trusting relationship to the individual. These are people whose voices are likely to be heard—siblings, spouses, or even adult children who have shown consistent care without resorting to pressure. It is often best to avoid including anyone with whom there is ongoing conflict or unresolved tension. Sometimes, it may be necessary to have honest conversations about why certain relatives are not included, focusing on the shared goal of supporting recovery.
Studies reveal that interventions are most effective when each family member’s message feels authentic and is delivered in a way that avoids blame. A facilitator can help the group practice these conversations in advance, ensuring everyone is prepared to respond with empathy and to avoid emotional triggers. With a carefully selected team, families can present a unified front and create a safe space for difficult conversations.5
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.

Preparing Communication That Breaks Through Hopelessness
Crafting Messages That Avoid Expressed Emotion Pitfalls
When preparing to communicate during an intervention, the way messages are crafted can make all the difference. Staging an intervention for depression requires family members to avoid the common pitfalls of "expressed emotion"—a term that covers criticism, hostility, or over-involvement. Studies have shown that high expressed emotion in families can actually increase relapse rates and make recovery harder for those with depression. Instead, messages should come from a place of empathy, respect, and shared concern.2
A helpful approach is to use "I" statements rather than accusatory language. This shifts the focus from blame to genuine observation and concern. Keeping messages short, specific, and non-judgmental is another best practice. For example, describing a recent change in behavior—like missing family dinners or neglecting hobbies—can open the door to conversation without triggering defensiveness.
"I’ve noticed you seem more withdrawn lately, and I care about your well-being."
Industry leaders find that rehearsing these statements with a professional beforehand helps reduce anxiety and maintains a supportive tone throughout the meeting. The table below highlights which communication styles help—and which harm—when staging an intervention for depression:
By intentionally crafting each message, families can reduce emotional barriers and create an environment where hope feels possible again. Next, the team can benefit from practicing responses to possible resistance or denial.2
Rehearsing Responses to Resistance and Denial
Rehearsing responses to resistance and denial is an essential part of staging an intervention for depression. Even with the most carefully crafted messages, it is common for individuals to respond with reluctance, skepticism, or outright refusal. Studies indicate that denial often stems from the deep sense of hopelessness and emotional exhaustion that accompanies depression, making it difficult for loved ones to see a path forward. As a result, families should prepare for these reactions in advance—both to avoid being caught off guard and to support the intervention’s steady momentum.6
A practical approach is for each team member to anticipate possible statements of resistance, such as “I don’t need help,” “Nothing will work for me,” or “This is just who I am.” Rehearsing calm, non-argumentative replies keeps the conversation grounded in empathy. Practicing these responses together helps everyone stay on script if emotions rise, reducing the risk of accidental escalation or withdrawal.
The table below outlines typical resistant statements and effective ways to respond:
By rehearsing these exchanges, families can approach the intervention with confidence and compassion, ready to gently guide their loved one toward accepting help. Next, attention shifts to creating a supportive physical and emotional setting for the intervention meeting itself.2
Conducting the Meeting When Staging an Intervention for Depression
Creating a Safe Environment for Difficult Conversations
Creating a safe environment is one of the most critical elements when staging an intervention for depression. The physical and emotional setting can either encourage openness or trigger defensiveness, so details matter. Industry experts recommend selecting a neutral, private location—somewhere free from distractions and with minimal risk of interruptions. This helps everyone stay focused and reduces the chance of the conversation feeling overwhelming or confrontational.3
Equally important is the emotional atmosphere. People respond best when they sense empathy, respect, and nonjudgmental support from those around them. Before the meeting, it helps for the intervention team to agree on ground rules to promote a sense of equality and safety:2
- Allow each person to speak without interruption.
- Avoid raised voices or accusations.
- Arrange seats in a circle instead of rows to reduce hierarchy.
Families can also provide comfort items, such as water or tissues, and let their loved one know they can take a break if things become too intense. The goal is to demonstrate care and patience, reinforcing that the conversation comes from concern, not criticism. With this foundation in place, the next section will address how to guide the conversation toward securing a commitment to professional evaluation.
Securing Commitment to Professional Evaluation
Securing a commitment to professional evaluation is often the most delicate phase when staging an intervention for depression. The conversation should center on compassion rather than pressure, keeping in mind that depression can cloud judgment and make decision-making feel overwhelming. Industry research highlights that individuals with depression are more likely to consider treatment when the path to evaluation is clear, concrete, and presented as a collaborative step, not a demand.3
Instead of ultimatums, families can offer specific options to reduce barriers and make the process less intimidating:
- Scheduling an appointment with a mental health clinician.
- Attending a first session together for moral support.
- Agreeing to an initial phone consultation.
It is also helpful to emphasize that professional evaluation is not a lifelong commitment—just a first step toward understanding what’s happening and exploring potential solutions. Studies reveal that with proper treatment, 80-90% of people living with depression experience significant improvement. This statistic can be reassuring for loved ones who feel hopeless or skeptical about recovery. If resistance surfaces, the team can revisit previously rehearsed empathic responses and reassure the individual that they are not alone in this process.

Ensuring Follow-Through and Long-Term Support
The real work begins after the initial crisis passes. Long-term support requires consistent check-ins, adaptive strategies, and a willingness to adjust the plan as circumstances evolve. Families often find that what worked in month one needs refinement by month three, and that is completely normal. Recovery isn't linear, and neither is the support structure surrounding it.
Establishing regular family meetings creates accountability and opens communication channels. These don't need to be formal sit-downs—sometimes a weekly coffee chat or Sunday dinner conversation works better. The key is consistency and creating a safe space where everyone can share concerns without judgment. Research shows that families who maintain structured communication report stronger relationships and better outcomes over time.
Professional support shouldn't disappear once immediate stability returns. A comprehensive support network often includes:
- Case Managers: Coordinate care across multiple providers and life demands.
- Recovery Companions: Offer real-time support during vulnerable moments.
- Behavioral Health Coaches: Help develop coping strategies that fit into busy schedules.
- Family Coaching Specialists: Guide communication patterns that strengthen rather than strain relationships.
Think of it like having a trusted advisory board for your family's wellbeing—professionals who understand the complexities of maintaining stability while managing careers, social obligations, and the privacy concerns that matter to high-achieving families. Whether it is adjusting communication strategies, addressing new stressors, or simply having someone to consult when questions emerge, sustained professional involvement makes a measurable difference.
When children are part of the family dynamic, professional support takes on additional dimensions. Parents need strategies to maintain their own stability while protecting their children's emotional wellbeing and sense of security. Family coaching specialists help parents determine what children need to know at different developmental stages, how to answer difficult questions honestly without oversharing, and ways to maintain routines that provide comfort during uncertain times. Co-parenting support becomes especially valuable when parents need to present a unified approach despite their own stress or differing perspectives. Services adapt to school schedules, extracurricular commitments, and the need for discretion in community settings where privacy matters most.
Building a support network beyond the immediate family also strengthens long-term success. This might include trusted friends, support groups, or community resources that align with the family's values and needs. The goal is creating multiple layers of support so no single person carries the entire burden of ensuring stability.
Conclusion
Supporting a loved one through behavioral health challenges requires patience, structure, and unwavering commitment to their well-being. The strategies outlined here—from establishing clear boundaries to coordinating professional resources—create a foundation that extends far beyond initial treatment. Families who build comprehensive support systems, rather than relying solely on their own resources, position themselves to provide meaningful assistance through the complexities that naturally arise.
The most effective support systems blend accountability with compassion, recognizing that sustainable change happens gradually. By maintaining consistent communication with treatment professionals, monitoring progress without micromanaging, and adjusting approaches as circumstances evolve, families create an environment where wellness can flourish. This balanced approach acknowledges both the seriousness of the situation and the dignity of the person working toward lasting change.
Specialized support exists that adapts to the realities of demanding lives—coordination that functions across time zones, discreet assistance that integrates into professional schedules, and expertise that travels wherever life requires. From the earliest conversations about change through years of sustained wellness, comprehensive care systems address not just immediate crises but the ongoing complexity of maintaining balance in high-pressure environments. These support structures can include everything from initial assessments and interventions to daily companionship and long-term life coordination, all calibrated to individual circumstances.
Long-term wellness depends on the entire family system adapting together, supported by professionals who understand the nuances of your particular situation. When everyone commits to their role—whether through therapy participation, boundary maintenance, or consistent presence—and when that commitment is reinforced by expert guidance tailored to your family's specific needs, the likelihood of lasting positive outcomes increases significantly. Consider whether your current support structure matches the complexity of what you are navigating. The journey toward sustained wellness may be intricate, but the right professional partnership makes it navigable.
Let's Create Lasting Change, Together
At Next Level Wellness & Behavioral Health, we provide premier concierge behavioral healthcare and highly personalized support for individuals and families navigating substance use, mental health challenges, eating disorders, complex life transitions, and more.
Our discreet, concierge, and expert-driven approach ensures dignity, compassion, and results-oriented care whether at home, in transit, or across multiple levels of treatment.
For support that meets you right where you are—anytime, anywhere—connect with us today.
Frequently Asked Questions
What happens if the person refuses help even after a professionally facilitated intervention?
If a loved one refuses help even after a professionally facilitated intervention, it can be discouraging, but it doesn’t mean hope is lost. Studies reveal that resistance is often part of the process—depression itself creates feelings of hopelessness and low motivation, making it hard to accept support right away. The most effective next step is to maintain open, caring communication without applying pressure or ultimatums, as these can increase distress and risk. Continue expressing concern and offering resources, but also respect their autonomy. If safety is a concern—such as talk of self-harm—seek immediate professional guidance. Sometimes it takes several conversations before someone is ready to accept help.5,6
How do we maintain boundaries while supporting someone who discontinues treatment prematurely?
Maintaining boundaries while supporting someone who stops treatment early is a common challenge after staging an intervention for depression. It helps to set clear expectations about what you can and cannot do—such as offering encouragement and sharing resources, but not taking responsibility for their choices. Studies show that about 50% of people discontinue antidepressant medication prematurely, so regular check-ins and gentle reminders are often needed. At the same time, families should avoid over-involvement or pressure, which can strain relationships and may actually increase resistance to treatment. Prioritizing self-care and seeking support for yourself—like family counseling or peer groups—can help maintain balance. Boundaries protect both your well-being and the dignity of your loved one.2,10
What are the next steps when initial treatment approaches don't produce improvement?
When initial treatment doesn’t lead to improvement, the next steps require both patience and flexibility. About 30% of individuals experience what’s called treatment-resistant depression, which means symptoms persist even after trying at least two types of antidepressant medication. In these cases, collaborating closely with a mental health professional is essential. Possible next steps include adjusting medication, combining medications, or incorporating evidence-based therapies like cognitive-behavioral therapy (CBT). Sometimes, advanced treatments such as electroconvulsive therapy (ECT) or other brain stimulation techniques are recommended. Ongoing family support and regular communication with care providers help ensure no one feels isolated or discouraged during this process. Each new step should be discussed as part of a shared effort toward recovery.10
How can family members recognize if their involvement is becoming counterproductive?
Family members can recognize if their involvement is becoming counterproductive by paying attention to both their own feelings and their loved one’s responses. If support starts to feel like pressure, if conversations often end in arguments, or if the person withdraws further after family attempts to help, these are key signs that boundaries might be crossed. Research shows that high levels of criticism, over-involvement, or emotional intensity from family—called “expressed emotion”—can actually increase the risk of relapse and worsen depression outcomes. Healthy support means offering encouragement and resources without trying to control every decision. When frustration or exhaustion becomes common, or when support feels more like monitoring than genuine care, it’s time to step back and consult a mental health professional for guidance.2
What timeline should we expect between intervention and visible signs of improvement?
After staging an intervention for depression, families often wonder how soon they’ll see signs of improvement. While some people experience small positive changes within the first few weeks of starting treatment, visible progress can take time. On average, it may take four to six weeks before noticeable shifts in mood, energy, or daily functioning occur after beginning therapy or medication. Research shows that with proper treatment, 80–90% of individuals with depression significantly improve, but early days often involve subtle changes rather than dramatic breakthroughs. Ongoing encouragement and patience from the support team are essential, since treatment response is gradual and setbacks are common. If improvement isn’t seen after several months, it’s wise to consult with a mental health professional about adjusting the approach.4,10
How do cultural considerations affect the intervention approach and treatment acceptance?
Cultural values and beliefs play a major role in both staging an intervention for depression and how treatment is accepted. In some cultures, depression may be seen as a private family matter or even a sign of weakness, which can increase stigma and make individuals less likely to accept outside help. Industry experts note that standard intervention models might not always recognize this, leading to less effective outcomes for families from diverse backgrounds. Adapting communication styles, language, and who participates in the intervention can help bridge these gaps. For example, including respected elders or community members may increase trust and treatment acceptance. Studies suggest that interventions are most successful when tailored to cultural expectations and when families acknowledge and address potential barriers to care.2
References
- Clinical Practice Guidelines for the management of Depression. PMC National Center for Biotechnology Information. https://www.pmc.ncbi.nlm.nih.gov/articles/PMC3893922/
- Family Interventions: Basic Principles and Techniques. PMC National Center for Biotechnology Information. https://www.pmc.ncbi.nlm.nih.gov/articles/PMC2830173/
- Depression (major depressive disorder) - Diagnosis and treatment. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/depression/diagnosis-treatment/drc-20356013
- Clinical Depression (Major Depressive Disorder): Symptoms. Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/9290-clinical-depression-major-depressive-disorder
- Depression Intervention: A Guide to When and How. Healthline. https://www.healthline.com/health/depression/depression-intervention
- How to Help Someone with Depression. HelpGuide. https://www.helpguide.org/articles/depression/helping-someone-with-depression.htm
- Depression Treatments for Adults. American Psychological Association. https://www.apa.org/depression-guideline/treatments
- Depression and Older Adults. National Institute on Aging. https://www.nia.nih.gov/health/depression-and-older-adults
- Warning Signs and Symptoms. NAMI. https://www.nami.org/About-Mental-Illness/Warning-Signs-and-Symptoms
- Treatment-resistant depression: definition, prevalence, detection and management. PMC National Center for Biotechnology Information. https://www.pmc.ncbi.nlm.nih.gov/articles/PMC3363290/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



