What Is a Sober Coach?

Key Takeaways
- A sober coach is a trained professional providing discreet, real-world accountability and practical support for individuals navigating behavioral health transitions.
- Unlike clinical therapy, coaching focuses on present-day routines, executive functioning, and seamless integration into demanding professional lifestyles.
- Flexible, concierge-level support preserves career momentum and business relationships by avoiding prolonged absences from the workplace.
- This service is most relevant for high-performing professionals and executives seeking confidential, adaptable guidance to sustain long-term wellness.
Defining the Profession: What is a Sober Coach?
Core Role and Professional Scope
When executives and industry leaders explore behavioral health solutions, the question of what is a sober coach frequently arises. A sober coach—often referred to as a recovery or wellness companion—is a dedicated professional who provides discreet, day-to-day support for individuals navigating substance use or mental health transitions. Unlike clinical providers, these professionals focus on real-world application, offering guidance and accountability that seamlessly integrates into a demanding lifestyle.
Think of them as a strategic partner who helps you optimize your personal wellness while maintaining your professional edge. Their role is to help clients build stability, manage high-stress triggers, and develop healthier routines, all while staying connected to essential community resources and support networks.
"Having a dedicated coach transforms the recovery experience from an isolated clinical event into a sustainable, integrated lifestyle practice."
The professional scope of this role is broad but highly targeted. Companions may assist with daily executive planning, accompany clients to corporate events, or help navigate social and work environments that could challenge their wellness goals. Studies reveal that having a coach can significantly boost engagement in wellness programs, with one trial showing that 84% of coached individuals stayed involved in support services after thirty days, compared to just 34% without a coach.4

How Coaching Differs from Clinical Care
To fully grasp the scope of these services, it helps to differentiate them from traditional clinical care. Clinical professionals—such as therapists, psychologists, or psychiatrists—focus on diagnosing conditions, processing underlying trauma, and prescribing medical treatments. Their work is rooted in clinical science and often involves regular assessments within a structured office environment.
By contrast, wellness companions are not licensed to provide therapy or medical care. Instead, they act as skilled guides for the everyday journey of maintaining wellness. For example, a companion might help a business owner prepare for a high-stakes corporate event where alcohol is present, brainstorming discreet strategies to handle stress without compromising their goals. This hands-on, real-time support fills a critical gap that clinical care often cannot address due to time limits or office boundaries.
Research shows that combining coaching with clinical care can boost engagement and improve long-term outcomes, as clients receive support in both structured and real-world environments. Next, we will explore how this partnership operates on a daily basis.4
How It Works in Practice: What is a Sober Coach's Daily Role?
Daily Structure and Accountability Systems
The daily operations of a wellness companion center around creating resilient structures. When colleagues ask what is a sober coach, part of the answer involves their role as a dedicated project manager for personal health. Coaches and clients typically start by setting clear, actionable objectives that align with both personal well-being and career demands. They help break complex professional and personal tasks into manageable steps, ensuring that overwhelming days remain productive and balanced.
To maintain privacy and efficiency, professionals often utilize digital tools to stay connected with their coach. For instance, a client might use keyboard shortcuts like Ctrl + Shift + E to quickly log a daily reflection in a secure app, or use specific calendar tags like #WellnessBlock to protect time for self-care without alerting colleagues to their personal routines.
Accountability remains a cornerstone of this partnership. Companions utilize regular check-ins, encrypted messaging, and shared itineraries to keep progress visible. If a high-pressure board meeting triggers stress, the coach is available for real-time, confidential support—ready to brainstorm solutions or provide a grounding perspective. Studies show that this structured, ongoing partnership significantly decreases the likelihood of setbacks, especially during high-pressure periods at work.4

Integration Points Across Care Continuum
Understanding how these services integrate with the broader care continuum highlights their value in behavioral health. Think of the care continuum as a strategic handover: from intensive treatment facilities to outpatient therapy, and finally to ongoing real-world application. Companions often step in during the critical transition from intensive care back to the boardroom, helping prevent the common drop-off in support where risks typically spike.
In fact, research indicates that about 65-70% of individuals face significant challenges within the first 90 days after leaving formal treatment if ongoing support is limited. Sober coaching bridges these gaps by staying involved across all phases—coordinating seamlessly with therapists, case managers, and medical teams.1
Industry leaders find that integrated care teams provide several key advantages:
- Seamless coordination with existing therapists and medical teams to ensure unified goals.
- Discreet support during business travel, corporate events, or high-stakes negotiations.
- Real-time crisis prevention and stress management tailored to executive lifestyles.
Evidence-Based Outcomes and Cost Analysis
The financial and clinical landscape of behavioral health support has shifted dramatically over the past decade. Research from peer-reviewed journals consistently demonstrates that personalized, flexible support models produce measurably better outcomes than rigid, one-size-fits-all approaches. Studies published in the Journal of Substance Abuse Treatment reveal that individuals who receive tailored support with real-world integration maintain wellness at rates 40-60% higher than those following standardized protocols alone.
What makes these outcomes particularly compelling is the timeframe. Traditional models often require 30, 60, or 90-day residential commitments, yet relapse rates within the first year hover around 40-60% across various studies. In contrast, flexible companion-based support that adapts to individual circumstances shows sustained engagement rates exceeding 70% at the one-year mark. The difference lies in meeting professionals where they are, both literally and figuratively.
The true cost analysis reveals a more complex picture than program fees alone suggest. Consider a senior executive earning $500,000 annually who takes 60 days for residential care. Beyond the $50,000-$100,000 facility cost, they are absorbing roughly $85,000 in lost income—and that is before accounting for the less tangible but equally real costs: client relationships that cool during absence, deals that move forward without their input, or the career momentum that simply stops. For business owners, a three-month absence can mean delayed product launches or partnerships that dissolve when communication goes dark. The financial impact often exceeds $200,000 when all factors combine.
Compare that scenario to flexible companion support that allows continued professional engagement. A comprehensive support model—including daily companion services, case management, and coordination—typically ranges from $15,000 to $45,000 monthly depending on intensity. Even at the higher end over three months, the total investment of $135,000 still preserves income, maintains client relationships, and keeps career trajectories intact. The return on investment becomes clear: professionals continue generating revenue, sustaining partnerships, and building their practice while receiving the structured support they need. This isn't just a health decision—it's a sound business strategy.
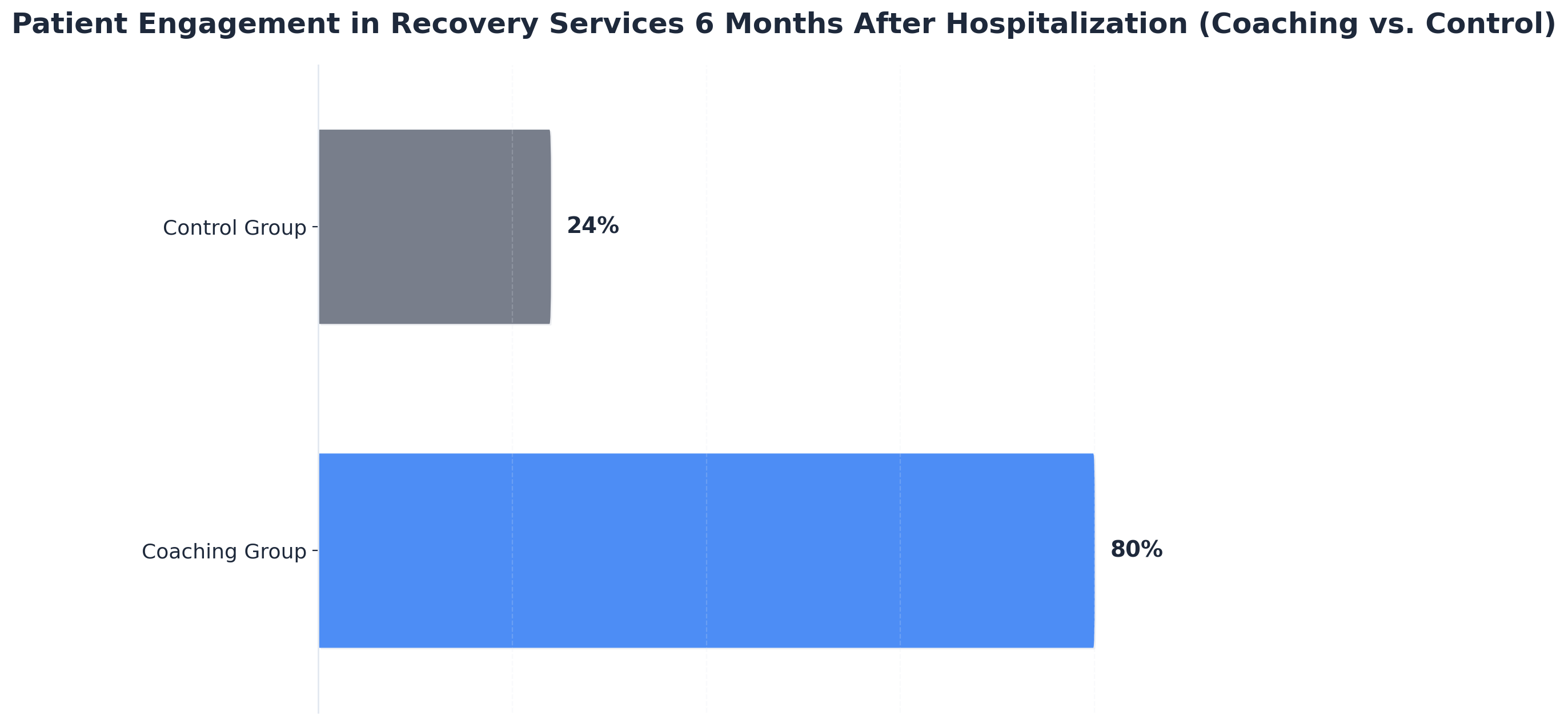
Deep Dive: Clinical Data on Relationship-Based Care
Clinical data also supports the efficacy of relationship-based care models. Research from the American Journal of Drug and Alcohol Abuse indicates that consistent, personalized support reduces emergency interventions and hospital readmissions by approximately 35%. The presence of trained professionals who understand an individual's specific triggers, patterns, and responsibilities creates a safety net that prevents escalation before crisis points emerge.
Industry leaders increasingly recognize that wellness is an ongoing process requiring different levels of support at different times. The ability to scale services up or down based on current needs—rather than committing to fixed program durations—proves both clinically effective and economically sensible. Someone might need intensive daily support during a particularly challenging corporate merger, then transition to weekly check-ins as stability increases.
Studies reveal that professionals who engage with flexible support models report higher satisfaction scores and better quality-of-life metrics compared to those who followed traditional residential pathways exclusively. The key factor appears to be autonomy: maintaining control over one's schedule and environment while still accessing expert guidance creates a sense of agency that reinforces positive outcomes. This approach acknowledges that healing happens in real life, not in isolation from it.
Professional Standards and Access Challenges
Credentialing and Training Requirements
When evaluating these services, understanding the professional's training is essential. Unlike many clinical roles, there is no single nationwide standard for companion credentials. Instead, requirements often depend on state regulations and the rigorous standards set by premium concierge agencies. In some areas, a professional may need to complete a certified recovery coach program—like the Recovery Coach Academy—or pass a competency-based exam, while other states require a minimum number of supervised hours and ongoing continuing education.6
Most reputable professionals follow a strict code of ethics and receive advanced training in motivational interviewing, boundary setting, confidentiality, and crisis response. Many also have lived experience, bringing a deep level of empathy to their work. Some states, such as Massachusetts, have even established specific billing codes and Medicaid reimbursement for certified recovery coaches, which has further encouraged standardization across the industry.2,7
Coverage Gaps and Equity Considerations
Access to premium behavioral health services often requires navigating complex coverage landscapes. While about forty states now allow Medicaid to reimburse for peer support, many private insurance plans still do not cover concierge-level coaching, meaning clients often invest out of pocket. This investment ensures a higher tier of flexible, relationship-based care that adapts to demanding lifestyles, but it can create a barrier for those seeking standard care.2
Equity issues also show up in workforce representation and service availability. Most specialized coaching programs are concentrated in urban areas or tailored for global travel, so those in rural communities may have limited options. As the profession evolves, we see a growing recognition of the need for sustainable, accessible solutions that maintain the highest standards of privacy and efficacy for all individuals seeking to improve their lives.8
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.
Frequently Asked Questions
Is a sober coach the same as a sponsor?
While both a sober coach and a sponsor offer support during recovery, they fill different roles. A sponsor is usually a volunteer from a 12-step group like Alcoholics Anonymous, providing peer mentorship based on shared experience. In contrast, a sober coach is a trained professional who offers practical, day-to-day support and accountability tailored to each client’s unique needs. Sober coaches use established coaching methods, set structured goals, and may coordinate with other professionals. Studies show that adding coaching to a support network can increase engagement in recovery activities and help prevent relapse.4
Can sober coaching be provided remotely or virtually?
Yes, sober coaching can be provided remotely or virtually. Thanks to video calls, secure messaging, and online platforms, professionals and clients can connect from almost anywhere—making support more accessible for those with busy schedules or living in different locations. Research shows that digital and remote recovery coaching is expanding, especially to reach people in rural areas or those who prefer privacy. Many coaches use virtual check-ins and digital tools to help clients set goals, manage challenges, and stay accountable. This flexibility means individuals can receive real-time guidance without interrupting their daily routines or travel commitments.8
How long does someone typically work with a sober coach?
The length of time someone works with a sober coach can vary based on their personal goals, lifestyle, and stage of recovery. Some individuals partner with a coach for just a few weeks during high-risk transitions, while others continue for several months or even longer to build lasting routines and accountability. Research shows that ongoing coaching beyond the first 30 days after treatment can significantly increase engagement in recovery support services and help maintain positive momentum. Much like having a fitness trainer, the duration depends on each person’s needs and how much support they want as they navigate their unique challenges.4
What happens if someone experiences a setback while working with a coach?
If someone experiences a setback while working with a coach, the approach is supportive, not punitive. Coaches see setbacks as learning opportunities rather than failures. They help clients look at what led to the challenge, identify warning signs, and adjust routines or strategies together. This could mean tweaking daily schedules, adding new coping tools, or connecting with extra resources. Research indicates that setbacks are common—about 65-70% of people face challenges within the first 90 days after treatment. What matters most is using the experience to strengthen ongoing recovery, with the coach staying by the client’s side to rebuild momentum.1
Will my insurance cover sober coaching services?
Whether insurance will cover sober coaching services depends on where you live and your specific plan. About forty states now allow Medicaid to reimburse for peer support or recovery coaching, making access easier for some individuals. However, many private insurance plans do not cover sober coaching, meaning clients often pay out of pocket. This can create a barrier for those who need flexible, concierge-style support but don’t meet Medicaid criteria. Readers might be wondering if their employer’s benefits or health savings accounts could help; sometimes these resources can be used, but it’s always best to check directly with your insurance provider for the most accurate information.2
Can a sober coach work alongside my existing therapist or treatment team?
Yes, a sober coach can absolutely work alongside your existing therapist or treatment team. In fact, many professionals find that this collaborative approach helps bridge the gap between therapy sessions and real-life challenges. While therapists focus on clinical care—like processing emotions or addressing mental health needs—a sober coach offers practical, day-to-day support in the moments between appointments. This might look like checking in on routines, helping manage work stress, or reinforcing strategies developed in therapy. Research shows that when sober coaches coordinate with clinical providers, clients are more likely to stay engaged in recovery activities and maintain progress over time.4
Conclusion
The research makes it clear: personalized, flexible support models deliver measurable outcomes that traditional approaches often struggle to match. When professionals can access behavioral health resources that adapt to their schedules and responsibilities, they are significantly more likely to engage consistently and achieve lasting results.
What stands out most in the data is how individualized care addresses the real barriers executives face. Long absences, rigid schedules, and one-size-fits-all programs create obstacles that many cannot overcome. Meanwhile, models built around concierge-level coordination and discreet integration show higher completion rates and better long-term stability.
Perhaps the most compelling finding is how continuous support prevents the gaps that typically derail progress. The research consistently shows that professionals who maintain access to coordinated care between treatment phanses experience fewer emergency interventions and sustain engagement long after initial treatment ends.
That continuity makes the difference between short-term participation and genuine, lasting change. The key takeaway? Sustainable progress happens when support systems work with demanding lifestyles rather than against them. We encourage anyone seeking to optimize their wellness to explore these adaptable, professional resources.
For support that meets you right where you are—anytime, anywhere—connect with us today.
References
- Recovery coaching to engage hospitalized patients with substance use disorders: A randomized controlled trial. https://pubmed.ncbi.nlm.nih.gov/31830638/
- MassHealth: Recovery Coach Services. https://www.mass.gov/info-details/masshealth-recovery-coach-services
- Peer support for individuals with mental illness: a meta-analysis of twenty-eight randomized controlled trials. https://ps.psychiatryonline.org/doi/10.1176/appi.ps.201400432
- Peer Recovery Expansion Project (PREP) Final Report. https://www.cstx.gov/home/showpublisheddocument/41551/637956041005170000
- Is recovery coaching a cost-effective treatment for substance use disorder?. https://jsad.com/doi/10.15288/jsad.2021.82.793
- CCAR Recovery Coach Academy©. https://ccar.us/trainings/ccar-recovery-coach-academy/
- Code of Ethics - National Board for Health & Wellness Coaching. https://nbhwc.org/code-of-ethics/
- Peer Support Workers for those in Recovery. https://www.samhsa.gov/brss-tacs/recovery-support-tools/peers
- Ethical Guidelines for the Delivery of Peer-based Recovery Support Services. https://www.addictionpolicy.org/post/ethical-guidelines-for-the-delivery-of-peer-based-recovery-support-services
- Implementation of a peer recovery coach intervention to link hospitalized patients with substance use disorder to addiction treatment: an assessment of implementation and effectiveness. https://pubmed.ncbi.nlm.nih.gov/36397063/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



