Recovery Associates Explained

Key Takeaways
- Recovery associates are specialized behavioral health professionals who utilize their own lived experience to provide non-clinical, concierge-level support for individuals navigating mental health and substance use challenges.
- They offer highly adaptable, discreet care that seamlessly integrates into demanding lifestyles, bridging the gap between clinical sessions and real-world application.
- These professionals maintain strict ethical boundaries while serving as a reliable extension of care for referring clinical professionals.
- This specialized support is most relevant for high-need or high-net-worth individuals requiring personalized, relationship-based assistance before, during, and after formal treatment.
What Recovery Associates Do in Behavioral Health
As referring clinical professionals, we understand that the journey to sustained wellness often requires support that extends beyond the traditional clinical setting. Recovery associates serve as a vital, professional extension of your care, offering concierge-level guidance for high-need or high-net-worth clients navigating complex behavioral health challenges. By drawing on their own lived experiences, these professionals provide a unique layer of support that helps clients translate clinical insights into daily, real-world success.
Recovery associates work collaboratively with clinical teams to ensure seamless, discreet care that adapts to a client's demanding lifestyle.

Core Definition and Scope of Practice
Unlike clinical staff such as therapists or psychiatrists, recovery associates do not diagnose, prescribe, or provide therapy. Instead, their primary function is to deliver non-clinical, peer-based support that feels adaptable and discreet. They help individuals set actionable goals, maintain motivation, and connect with premium community resources. Think of them as specialized navigators—individuals who have successfully traversed similar paths and now provide expert, real-world companionship as clients work toward lasting wellness.
The scope of practice for these professionals is clearly defined to complement your clinical work. They listen without judgment, share practical coping strategies, and help clients build robust skills for daily living. Their support might include accompanying clients to appointments, facilitating safe transport, or helping with life coordination tasks that promote stability. For example, an associate might help a client create a sustainable daily routine or identify environmental triggers during a business trip. However, they never replace clinical treatment, and they are rigorously trained to recognize when a client needs to be referred back to medical or mental health professionals.1
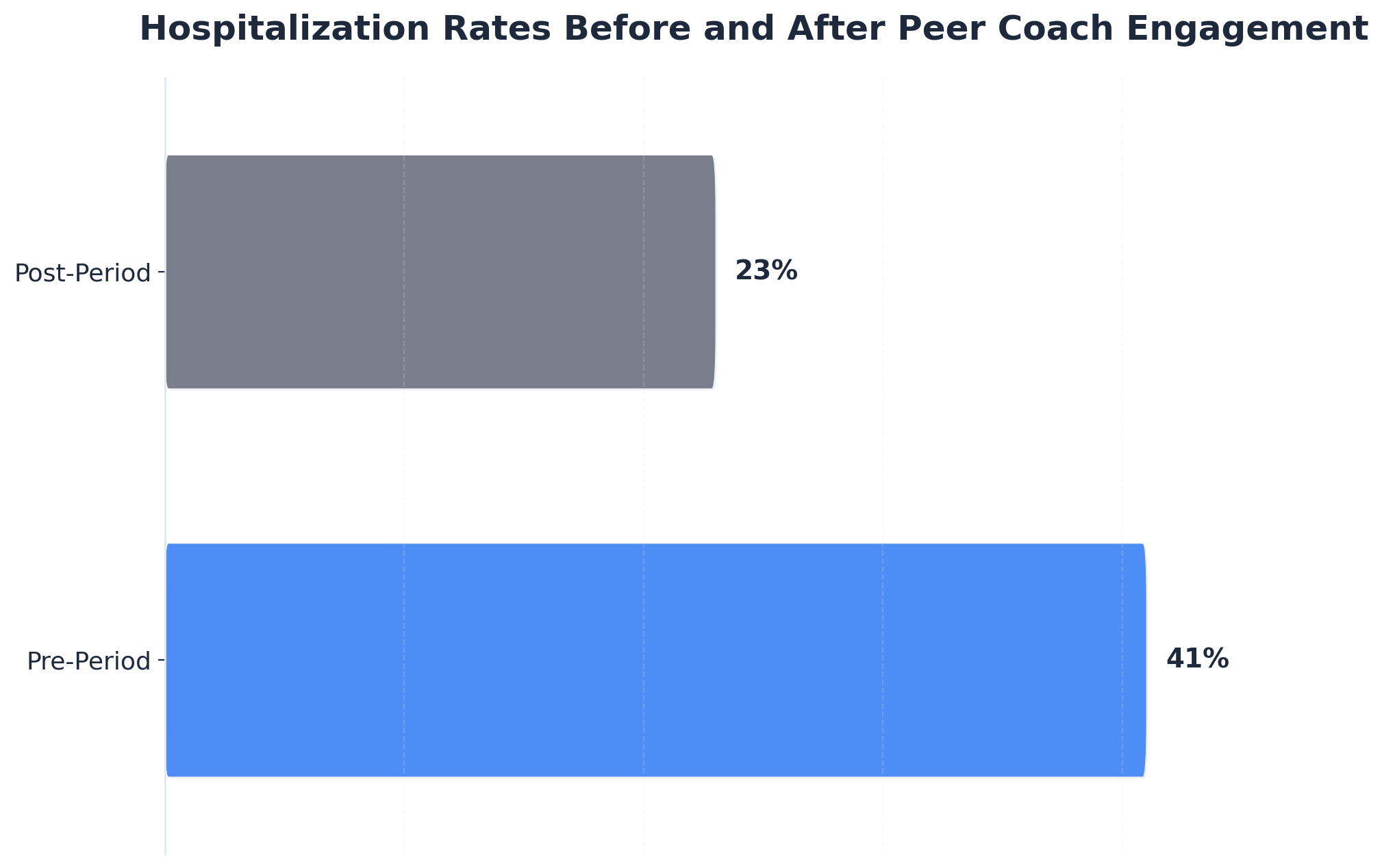
Research shows that the involvement of these specialized companions is linked to higher engagement in treatment and fewer hospitalizations, with one program showing a drop in hospitalization rates from 41% to 23% after clients accessed peer support. Understanding the foundation of this role sets the stage for exploring the unique value that lived experience brings to the behavioral health workforce.3
Lived Experience as Professional Credential
Lived experience is not just a personal story for these professionals—it is a core professional credential. Unlike most behavioral health roles, recovery associates qualify for their positions specifically because they have navigated their own journey of healing. This allows them to build trust rapidly with affluent or high-profile clients, who often feel more comfortable opening up to someone who truly understands the nuances of their struggles without clinical detachment.
Consider how a seasoned executive mentor who has already overcome industry challenges can guide a newcomer through unknown territory. Recovery associates use their past struggles and successes as a bridge, offering hope and practical strategies that are proven to work in real life. Their experience is an essential tool for building authentic connections, reducing stigma, and demonstrating that sustainable change is possible.
"The integration of lived experience into behavioral healthcare transforms abstract clinical directives into actionable, daily achievements for clients."
Readers might be wondering how this shared background translates into measurable outcomes. Industry leaders find that seeing someone who has faced similar hurdles and found stability can be a turning point for those early in the process. Clients with access to this level of personalized support are more likely to stay involved in treatment and less likely to experience acute crises. As the behavioral health field develops pathways to formally recognize and train these professionals, we ensure their lived experience is paired with strong professional standards.3
Evidence Base for Recovery Associates and Peer-Driven Support
The effectiveness of peer-driven support has been extensively documented across multiple research studies and real-world implementations. Clinical trials consistently demonstrate that individuals who engage with mutual aid services show improved treatment retention rates, reduced relapse episodes, and enhanced overall quality of life compared to those receiving traditional care alone. These outcomes reflect the unique value that shared lived experience brings to the healing process.
A landmark study published in the Journal of Substance Abuse Treatment followed over 2,000 participants for three years and found that those who participated in peer-facilitated programs were 27% more likely to maintain continuous wellness than control groups. The research highlighted that these relationships created accountability structures that felt less clinical and more authentic, leading to greater engagement. Participants reported feeling understood in ways that traditional therapeutic relationships sometimes couldn't replicate, particularly during moments of crisis or self-doubt.
The evidence extends beyond substance use challenges. Mental wellness companions have shown remarkable results in reducing psychiatric hospitalizations and emergency department visits. Data from community programs indicates that peer-led interventions can decrease hospital readmissions by up to 40% while simultaneously improving medication adherence and treatment plan compliance. These clinical improvements stem partly from the reduced isolation and enhanced social support that peer relationships provide.
Research reveals that peer-based support creates measurable improvements in social connectedness. Studies tracking social integration metrics show that participants in peer-driven programs develop broader, wellness-oriented social networks. These psychological shifts prove particularly valuable for high-net-worth and high-need clients who may struggle to connect with traditional support structures that don't align with their lifestyle, professional demands, or privacy requirements. The discretion and adaptability of personalized support addresses barriers that often prevent successful individuals from accessing ongoing assistance.
From a clinical perspective, these relationships serve as a force multiplier for professional interventions. Therapists and psychiatrists report that clients engaged in peer-driven initiatives demonstrate greater insight into their own patterns and show increased willingness to implement therapeutic recommendations. Key benefits observed by clinical teams include:
- Real-time support during vulnerable moments when professional care isn't immediately accessible.
- Seamless life coordination that reduces environmental stressors.
- Enhanced communication between the client and their primary care team.
The evidence base has grown strong enough that major healthcare systems and accrediting bodies now recognize peer-facilitated support as an evidence-based practice. Organizations including SAMHSA and the National Institute on Drug Abuse have published guidelines endorsing the integration of lived-experience support into comprehensive care models. This institutional validation reflects decades of research demonstrating that assistance from those with shared backgrounds produces tangible, measurable outcomes.
Insight Beyond Treatment
At Next Level Wellness & Behavioral Health, we believe meaningful change starts with perspective, not just protocols.
That philosophy is directly led by Amanda Marino, whose voice in behavioral health extends beyond clinical settings into leadership, culture, and personal growth.
Through keynote speaking and live events, Amanda explores the deeper themes that show up in recovery, family systems, and life transitions: authenticity, resilience, accountability, and the courage to change. Her work invites audiences to move past labels and into honest conversations that create lasting impact.
Professional Standards and Workforce Integration
When integrating these professionals into your practice's workflow, clear communication and documentation are essential. For example, clinical teams might use specific EHR tags to track peer interactions. Entering Ctrl + F to search for peer_support_notes in a client's file can quickly pull up their daily progress. A standard documentation snippet from a recovery associate might look like this:
Certification Pathways and Training Requirements
To ensure quality and consistency, recovery associates pursue formal certification pathways before joining behavioral health teams. While requirements vary by state, nearly all states now offer a credentialing process for peer support professionals. This typically involves a combination of lived experience, completion of approved training courses, and supervised hours in the field. Think of it as earning a specialized professional license: it requires both real-world practice and rigorous classroom learning to qualify.
For instance, to become a Certified Peer Recovery Specialist (CPRS) in Maryland, candidates must complete 46 hours of core training plus 500 hours of supervised, practical experience. Continuing education is also required, with at least 50 hours every two years across key domains like advocacy, ethical responsibility, mentoring, and harm reduction. These rigorous standards help professionals remain effective and up to date with best practices.2
Training programs cover essential topics—confidentiality, cultural responsiveness, motivational interviewing, and self-care—equipping professionals to handle the wide range of challenges their clients may face. Credentials like the Recovery Coach Professional (RCP) designation are gaining traction across state lines, supporting career mobility and setting a benchmark for quality.6
Studies reveal that certification not only boosts client safety but also helps these professionals earn trust from clinical teams, making them highly valued partners in integrated care settings. Next, we’ll explore how clear ethical boundaries and defined roles ensure this support remains safe, effective, and sustainable.7
Ethical Boundaries and Role Clarity
Ethical boundaries and clear role definitions are at the core of safe, effective support in behavioral health. Recovery associates are not clinicians—they do not diagnose, provide therapy, or manage medications. Instead, they focus on building trusting relationships and sharing practical strategies drawn from their own journeys. A helpful analogy is thinking of them as experienced teammates: they offer encouragement, share what worked for them, and help clients find their own path, but they never take over the physician’s playbook.
Setting and maintaining boundaries can be challenging, especially since these professionals connect with clients through shared life experiences. Professional codes of conduct emphasize the importance of avoiding dual relationships, such as friendships or romantic involvement, which could blur the line between professional support and personal life. Consistent supervision and ongoing training help them spot when they’re stepping outside their role or being asked to do tasks better suited for clinical staff.7
When recovery associates have well-defined roles, clinical teams are more likely to trust and collaborate with them, and clients benefit from clear, coordinated care. As the field grows, organizations are refining policies and job descriptions to reduce confusion and promote ethical, sustainable support. This ongoing commitment to role clarity paves the way for addressing workforce challenges and ensuring high-tier service delivery.7
Current Challenges Facing Recovery Associates in the Field
Despite the growing evidence supporting peer-driven care, the field faces significant obstacles that can impact service quality and sustainability. Workforce development remains one of the most pressing concerns. Many specialists enter the field with lived experience but require ongoing formal training in boundaries, ethics, and professional communication. This gap can create challenges when working alongside clinical teams who expect consistent documentation and strict adherence to treatment protocols.
Standardization presents another complex issue. While the highly personalized nature of these services is its greatest strength, the lack of uniform training requirements across states makes it difficult for referring professionals to assess qualifications. Some regions require extensive certification programs, while others have minimal oversight. This inconsistency can leave clinical teams uncertain about the scope and reliability of peer-delivered interventions.
Burnout and retention also threaten the field's growth. Specialists often work with individuals facing intense crises while managing their own wellness journeys. Without adequate supervision, reasonable caseloads, and professional development opportunities, many talented individuals leave the field prematurely. Organizations investing in ongoing training and clinical supervision see significantly better retention rates.
Best Practices for Vetting Partner Organizations
When evaluating organizations as a professional extension of your practice, look for specific indicators of quality. Seek providers with structured supervision protocols and documented training programs that go beyond basic certification. Organizations committed to ongoing professional development demonstrate the reliability your high-need clients require.
Integration into clinical settings continues to evolve. Some treatment facilities still view these services as supplementary rather than essential, leading to inadequate compensation and limited career advancement opportunities. When peer professionals lack institutional support, continuity of care suffers, and the seamless coordination that benefits clients becomes harder to maintain.
Assess a provider's integration capabilities by asking about communication systems, documentation standards, and how they coordinate with clinical teams to ensure seamless transitions. Finally, examine their approach to staff retention and wellness—providers who invest in reasonable caseloads and support their team's own journeys are better positioned to deliver the stable, long-term relationships that make this support truly effective. These concrete markers separate well-structured organizations from the rest, helping you confidently refer clients to services that will genuinely complement your clinical work.
Frequently Asked Questions
What's the difference between a recovery coach and a peer support specialist?
The titles “recovery coach” and “peer support specialist” are often used in behavioral health, but they have subtle differences. Both roles are types of recovery associates who use their lived experience to support others, but a peer support specialist usually works within a certified, structured program and follows set guidelines laid out by their state or organization. A recovery coach, on the other hand, may have more flexibility, focusing on goal-setting, motivation, and helping clients develop recovery plans. Think of a peer support specialist as following a playbook, while a recovery coach adapts strategies to meet each person’s needs. Both roles are grounded in non-clinical, peer-based support.1
Can recovery associates provide clinical services or therapy?
Recovery associates are not permitted to provide clinical services or therapy. Their role is focused on non-clinical, peer-based support—think of them as experienced guides who listen, encourage, and offer practical strategies from their own recovery journeys. Unlike therapists, counselors, or doctors, recovery associates do not diagnose conditions, prescribe medications, or conduct therapy sessions. Instead, they help clients set goals, build daily living skills, and connect with community resources. When a client needs clinical care, recovery associates are trained to refer them to the appropriate licensed professionals. Clear boundaries like these help keep both the client and the recovery associate safe and supported.1
Does Medicaid cover peer recovery support services in all states?
Medicaid does not cover peer recovery support services in every state, but access is steadily expanding. States have the option to include these services under their Medicaid plans, and most now do, but coverage details and requirements can look quite different depending on where you are. For example, some states reimburse for a broad range of peer services, while others may have stricter limits or require additional certifications. Research shows that this patchwork can create confusion for both clients and referring professionals, especially when coordinating care across state lines. As Medicaid policies evolve, it’s important to check your state’s specific guidelines for recovery associates and peer support coverage.8
How do recovery associates maintain boundaries while using their lived experience?
Recovery associates maintain professional boundaries by following clear ethical guidelines and ongoing supervision. While sharing lived experience helps build trust, they’re trained to focus on what is helpful for the client’s recovery, not to process their own stories or form personal friendships. A good analogy is that of a guide on a hiking trail: they share tips and warn of obstacles based on their own journey, but don’t walk off the path with those they’re helping. Regular training and supervision help recovery associates recognize when a conversation or relationship is drifting into unsafe territory, ensuring safety for both parties.7
What impact have recent federal funding cuts had on peer support programs?
Recent federal funding cuts have had a significant impact on peer support programs across the country. With reductions of about $350 million in addiction and overdose prevention funding and layoffs at key agencies like SAMHSA, many organizations have struggled to maintain or expand their recovery associates teams. These cuts have led to hiring freezes, fewer training opportunities, and in some cases, the closure of peer support programs. For clients and referring professionals, this means fewer available resources and longer wait times for much-needed support. Maintaining stable funding is crucial for the continued growth and effectiveness of peer support services.8
Are recovery associates effective for clients with co-occurring mental health conditions?
Yes, recovery associates are effective for clients with co-occurring mental health conditions. Research shows that peer-driven support isn’t limited to just substance use—benefits extend to individuals facing both substance use and mental health challenges. For example, clients engaging with recovery associates are more likely to stay connected to care, experience fewer hospitalizations, and develop stronger self-management skills, even when mental health symptoms are present. Think of recovery associates as knowledgeable teammates who offer encouragement and real-world strategies, making it easier for clients to navigate complex behavioral health needs. Their unique role helps bridge gaps in traditional care models.3
Conclusion
The behavioral health field stands at a pivotal moment. While challenges around standardization and professional recognition persist, the evidence supporting peer-delivered services continues to grow stronger. Clinical professionals increasingly recognize that traditional therapeutic approaches, while essential, don't always address the practical, day-to-day realities their clients face when striving for long-term wellness.
Research shows that these specialized services fill critical gaps in the continuum of care—offering real-world guidance, modeling sustainable habits, and providing the kind of relatable connection that complements clinical treatment. As the field matures, the focus is shifting from whether these services work to how they can be most effectively integrated into comprehensive, concierge-level care plans.
For professionals working with high-need clients, consider this level of support when clinical progress stalls due to practical implementation challenges, when clients struggle with real-world scenarios between sessions, or when the transition from structured treatment to independent living feels overwhelming. The most successful outcomes emerge when clinical expertise and lived experience work in tandem. For high-net-worth clients especially, discretion and lifestyle integration become paramount—support that adapts to demanding schedules, travel requirements, and privacy concerns can bridge the gap between clinical recommendations and daily reality.
Moving forward, the clinical-peer partnership represents an essential component of comprehensive support that extends professional guidance into the moments that matter most. If you or someone you are treating is navigating mental health or substance use challenges, remember that compassionate, professional help is available. We encourage reaching out to specialized concierge services to build a comprehensive, supportive care team that fosters lasting wellness.
For support that meets you right where you are—anytime, anywhere—connect with us today.
References
- Peers Supporting Recovery from Substance Use Disorders. https://www.samhsa.gov/sites/default/files/programs_campaigns/brss_tacs/peers-supporting-recovery-substance-use-disorders-2017.pdf
- Certified Peer Recovery Specialist. https://www.mabpcb.com/certified-peer-recovery-specialist-cprs
- What is the Evidence for Peer Recovery Support Services?. https://www.recoveryanswers.org/research-post/what-is-the-evidence-for-peer-recovery-support-services/
- Initial Evaluation of Peer Recovery Coach Program in Large Hospital System. https://www.recoveryanswers.org/research-post/initial-evaluation-peer-recovery-coach-program-large-hospital-system/
- Barriers and Facilitators to Peer Support Services for Patients. https://pmc.ncbi.nlm.nih.gov/articles/PMC9009995/
- How to Become a Peer Support Specialist. https://mhanational.org/resources/how-become-peer-support-specialist/
- Peer Recovery Coaching Standards for Professional Practice. https://www.iaprss.org/wp-content/uploads/2023/05/PRC-Standards-for-Practice-Publication.pdf
- Frequently Asked Questions on Medicaid and CHIP Coverage of Peer Support Services. https://www.medicaid.gov/federal-policy-guidance/downloads/faq06052024.pdf
- Trump Cuts Have Decimated SAMHSA. https://www.statnews.com/2025/10/30/samhsa-grant-cuts-staff-reductions-impact-analyzed/
- Factors Associated with Peer Recovery Support Specialists' Intent to Remain or Leave. https://pubmed.ncbi.nlm.nih.gov/39666482/
A Voice Shaping the Conversation
The topics explored here—change, self-awareness, recovery, and growth—are the same themes Amanda Marino brings to audiences nationwide through speaking engagements and live events.
Known for her appearances on A&E’s Intervention and Digital Addiction, Amanda speaks to organizations, communities, and leadership teams about navigating adversity, embracing vulnerability, and building lives rooted in purpose. Her message resonates far beyond treatment, offering insight that applies to families, professionals, and anyone standing at a crossroads.
.svg)



